Musculoskeletal or neurological condition affecting mobility or function.
If you've been diagnosed with adult torticollis, you're dealing with a condition that affects far more than just your neck muscles. Adult torticollis, medically known as cervical dystonia (CD), is a neurological movement disorder where your neck muscles contract involuntarily, causing your head to twist, tilt, or turn into abnormal positions.
This isn't simply a "stiff neck" – it's the most common form of focal dystonia in adults, affecting your quality of life in ways that extend far beyond physical discomfort.
What's Actually Happening in Your Body
When you have cervical dystonia, your brain sends faulty signals to your neck muscles, causing them to contract when they shouldn't. These contractions are:
Physical Signs You Might Experience
Your head may deviate in multiple directions simultaneously:
The Pain Reality
Pain isn't just a side effect – it's a major component of this condition. Research shows that up to 70% of patients experience pain, typically described as:
Additional Symptoms That Matter
Beyond the obvious neck issues, you might also experience:
Understanding what's involved in your torticollis helps explain why treatment requires a comprehensive approach.
Your Neck's Muscular System
The involuntary contractions primarily affect your cervical (neck) muscles, including:
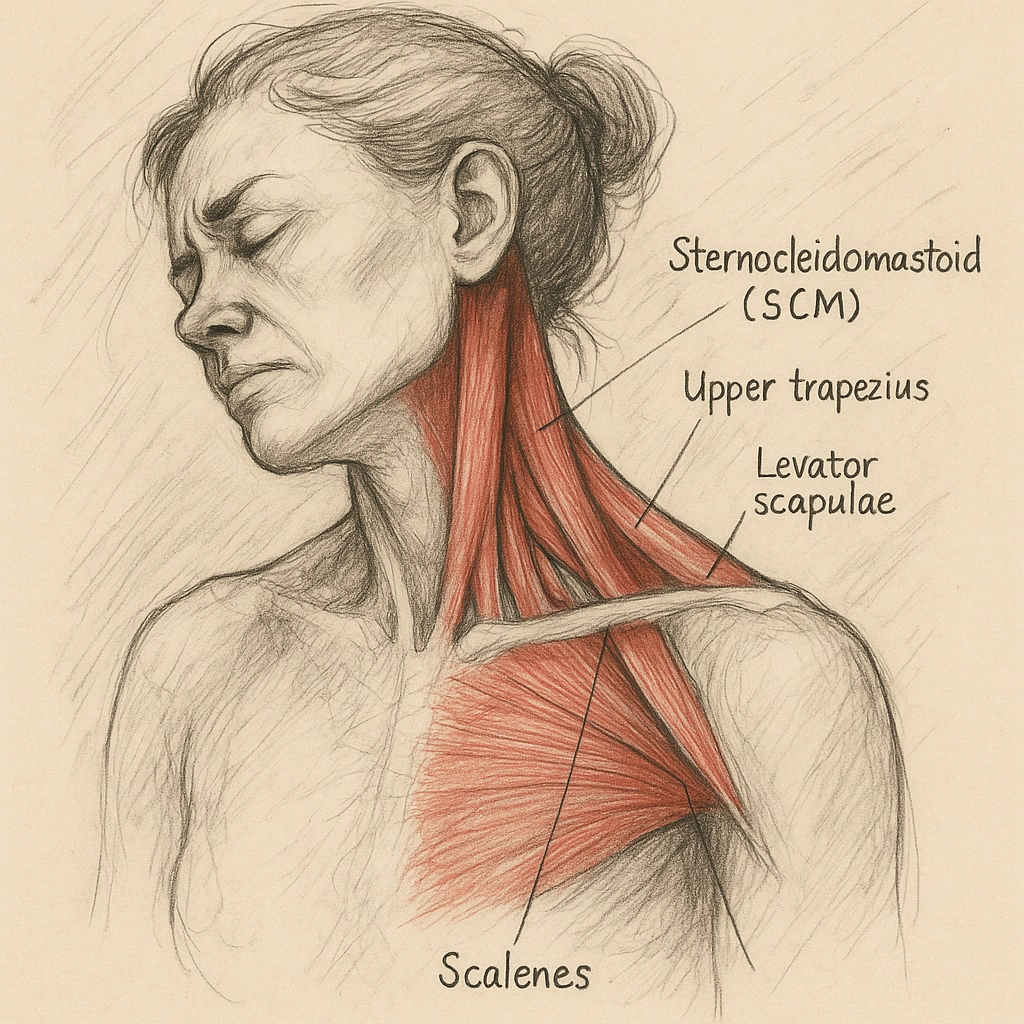
What makes this condition particularly challenging is the co-contraction phenomenon – when muscles that should work in opposition (agonist and antagonist) contract simultaneously, which voluntary movement can actually make worse.
Joint and Structural Involvement
Your cervical spine's facet joints may become irritated or dysfunctional, leading to:
The Neurological Component
This is fundamentally a brain-based condition involving:
Postural Control Systems
Your condition affects multiple body systems:
Understanding the "Why" Behind Your Condition
Most cases of adult torticollis are classified as idiopathic, meaning the exact cause remains unknown. However, research has identified several potential contributing factors:
Immediate Triggers
Neurological Factors
Individual Risk Factors
Research shows certain factors increase your likelihood of developing this condition:
The good news is that physiotherapy offers significant benefits for managing adult torticollis, whether you're dealing with acute symptoms or chronic cervical dystonia. Treatment approaches vary based on your specific situation and symptom duration.
Recover faster, move better, and feel stronger with expert physiotherapy. Our team is here to guide you every step of the way.

Immediate Pain and Spasm Relief
When your symptoms first appear or during acute flare-ups, the focus is on reducing pain and muscle tension:
Manual Therapy Techniques
Gentle Movement Introduction
Education and Postural Guidance
Restoring Function and Control
As your acute symptoms stabilize, treatment shifts toward rebuilding normal movement patterns:
Range of Motion and Mobility
Muscle Re-education
Sensorimotor Training
Comprehensive Dystonia Management
For chronic cervical dystonia, physiotherapy works best as part of a multidisciplinary approach:
Advanced Exercise Programs
Specialized Techniques
Integration with Medical Management
Acute Torticollis Recovery
Subacute Phase Outcomes
Chronic Dystonia Management

Essential Do's for Recovery
✅ Start gentle movement early – Begin appropriate exercises as soon as symptoms allow✅ Use heat and self-massage – Apply heat therapy and gentle self-massage for tension relief✅ Maintain excellent posture – Focus on proper alignment throughout your day✅ Commit to daily exercises – Include neck strengthening and postural exercises in your routine✅ Stay active – Avoid prolonged periods of inactivity✅ Manage stress – Incorporate stress-reduction techniques as symptoms can worsen with stress
Critical Don'ts to Avoid
❌ Don't immobilize unnecessarily – Avoid prolonged use of neck braces unless specifically prescribed❌ Don't rely on passive treatments alone – Combine massage and manual therapy with active exercises❌ Don't fear movement – Gentle, guided motion is therapeutic and necessary for recovery❌ Don't ignore ergonomics – Poor workplace setup can perpetuate your condition❌ Don't delay treatment – Early intervention typically leads to better outcomes
"Is it safe to move my neck with this condition?"
Absolutely. Gentle, guided movement is not only safe but essential for recovery. Research consistently shows that active exercises improve neck strength, range of motion, and reduce the effort required for head movement. The key is working with a qualified physiotherapist who can guide you through appropriate progressions.
"Do I need imaging like X-rays or MRI?"
While imaging may be recommended by your physician to rule out structural problems, the diagnosis of cervical dystonia is typically made by clinical examination, often by a movement disorder specialist. Your physiotherapist will focus on functional assessment and treatment regardless of imaging findings.
"Can stress or poor sleep really cause torticollis?"
Stress and sleep disturbances are recognized as significant factors that can worsen symptoms. Mental and physical stress can aggravate cervical dystonia symptoms, which is why stress-reduction techniques like progressive muscle relaxation, yoga, and proper sleep hygiene are important components of comprehensive treatment.
"Will my torticollis come back?"
"How long before I see improvement?"
Timeline varies by individual and condition type:
Adult torticollis, whether acute or chronic, is a manageable condition with the right approach. The key to success lies in:
Remember, this condition affects far more than just your neck – it impacts your entire quality of life. With proper understanding, treatment, and commitment to your recovery program, you can regain control and return to the activities that matter most to you.
Your journey to recovery starts with the first step. Work with your healthcare team to develop a personalized treatment plan that addresses your specific needs and goals.
Don't let adult torticollis limit your activities or affect your daily life. Our experienced team is ready to help you build a strong foundation for lasting recovery from this complex neck condition.
Book Your Specialized Torticollis Assessment Today:
Serving communities across Thornhill, Langstaff, Newtonbrook, Willowdale, North York, Markham, Richmond Hill, Concord, and North Toronto.
Just minutes from Yonge Street on Steeles Avenue West, our clinic offers flexible scheduling to support your recovery journey.
Whether you're navigating acute torticollis symptoms or chronic cervical dystonia, our evidence-informed approach can help you move with confidence and regain control of your head and neck positioning. Contact us today to take the first step toward empowered, supported living with torticollis.
Explore the latest articles written by our clinicians