
Musculoskeletal or neurological condition affecting mobility or function.
Benign Paroxysmal Positional Vertigo, commonly called BPPV, is the leading cause of vertigo worldwide. If you're experiencing sudden spinning sensations when you move your head in certain ways, you're not alone – BPPV affects millions of people and is highly treatable.
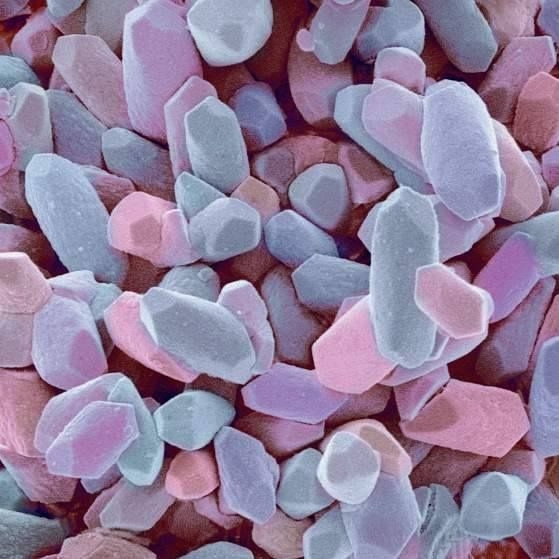
To understand BPPV, imagine your inner ear as a sophisticated navigation system with tiny crystals that help you maintain balance. Here's what happens:
Normal Function: Inside your inner ear, microscopic calcium carbonate crystals called otoconia (think of them as tiny pebbles) are normally attached to a gel-like membrane in an area called the utriculus. This structure acts like a natural level, helping your brain understand which way is up.
When BPPV Develops: These crystals become dislodged – often without any clear reason – and float into one of three semicircular canals (curved tubes filled with fluid). The posterior canal, located at the back, is most commonly affected, though the horizontal canal can also be involved.
The Problem: Once these loose crystals enter a semicircular canal, they act like debris in a drain. When you move your head, they shift around and create abnormal fluid movement. This sends false signals to your brain about head movement, creating the intense spinning sensation we call vertigo.
Canalithiasis (The Current Understanding): The crystals float freely within the canal, moving like a "plunger" when your head changes position. This is the most widely accepted explanation and accounts for most BPPV cases.
Cupulolithiasis (Less Common): The crystals stick to the cupula (a sensor at the end of the canal), making it heavier and more sensitive to gravity. This theory explains some cases that behave differently from typical BPPV.
BPPV creates a very specific pattern of symptoms that most patients describe similarly:
The Spinning Sensation: You experience intense vertigo – not just dizziness, but a clear sensation that either you or the room is spinning. This isn't a vague feeling; it's often dramatic and unmistakable.
Sudden Onset: The vertigo hits suddenly when you move your head in specific ways. There's typically no warning – one moment you're fine, the next you're experiencing intense spinning.
Brief but Intense: Episodes usually last less than a minute, often just 10-20 seconds. However, these brief moments can feel much longer when you're experiencing them.
BPPV symptoms are predictably triggered by specific movements:
Nausea and Vomiting: The intense spinning often triggers nausea, which can last for hours even after the vertigo stops.
Eye Movements: During an episode, your eyes may move involuntarily in a specific pattern (called nystagmus). This often includes both rotational and up-and-down movements.
Unsteadiness: You might feel off-balance or unsteady, particularly immediately after an episode.
Anxiety: The sudden, intense nature of BPPV can be frightening, leading to anxiety about when the next episode will occur.
It's important to understand that BPPV:
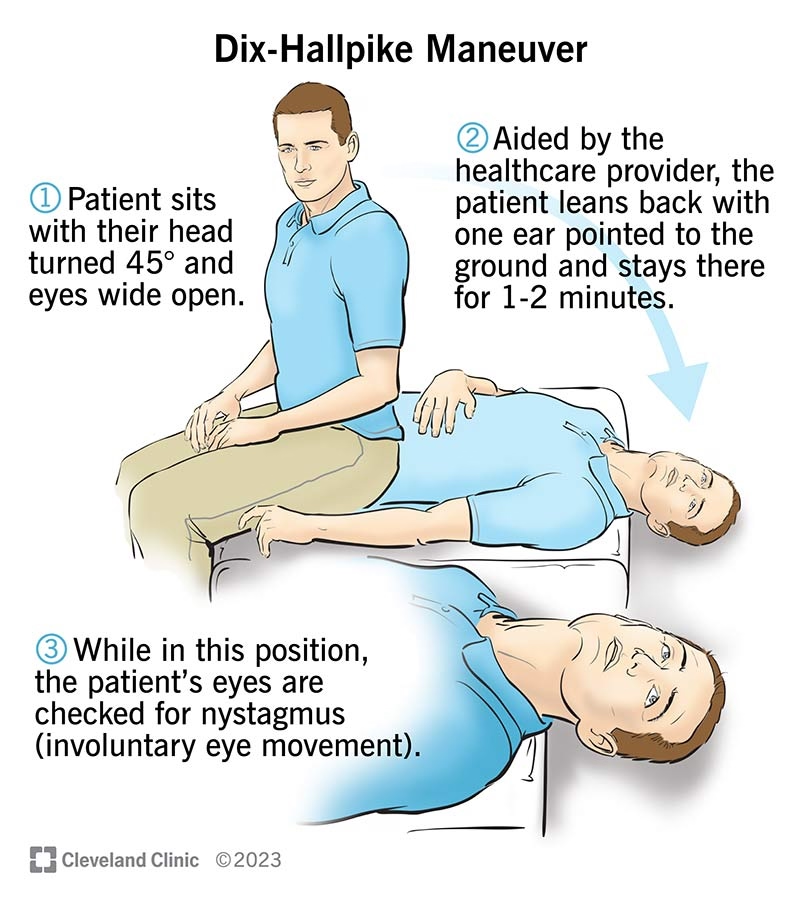
Your healthcare provider can diagnose BPPV right in the office using a simple but specific test called the Dix-Hallpike maneuver:
What Happens: You'll be moved quickly from sitting to lying down with your head turned and slightly extended. If you have BPPV, this will trigger vertigo and characteristic eye movements.
What to Expect: The test recreates your symptoms, so you'll likely experience vertigo during the test. This confirms the diagnosis.
Key Features of a Positive Test:
For horizontal canal BPPV, your provider might use the "supine roll test," where you lie down and turn your head side to side.
In most cases, no additional testing like MRI or CT scans is needed – the physical examination is sufficient for diagnosis.
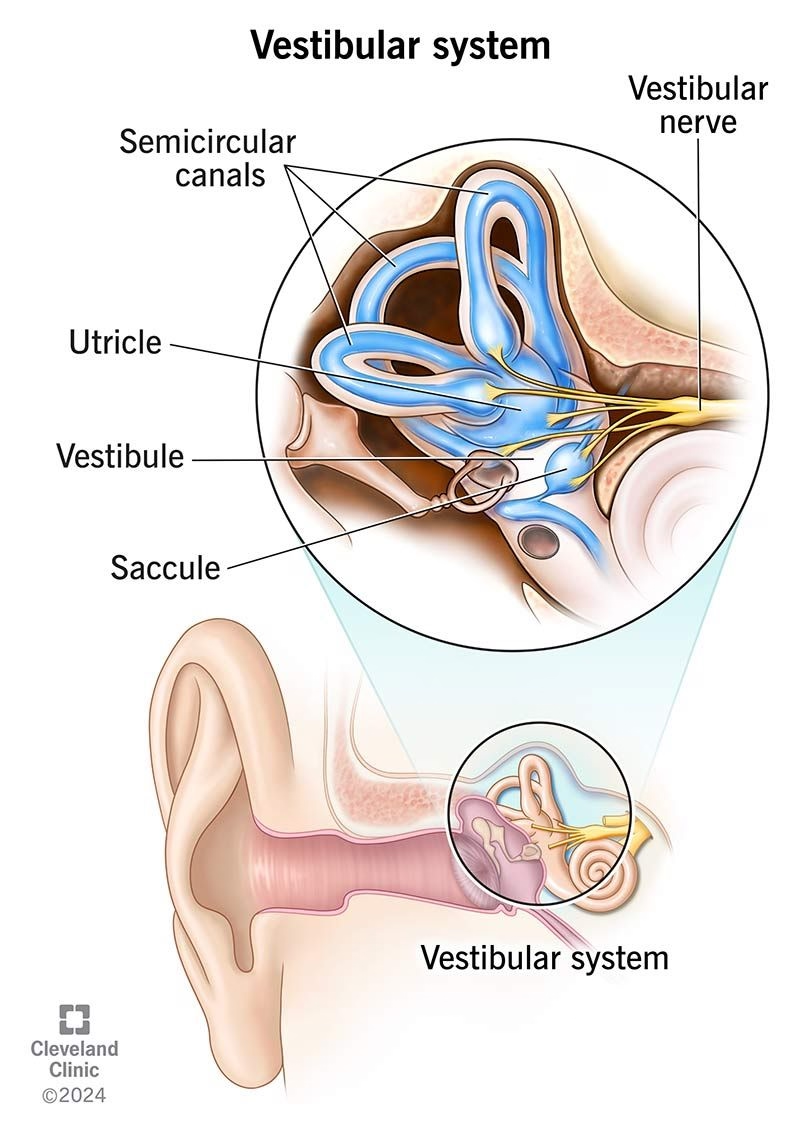
Understanding why BPPV affects you so dramatically requires learning about your inner ear – one of the most sophisticated balance systems in nature. Think of it as your body's personal GPS and gyroscope, constantly working to keep you oriented and steady.
Located deep within the temporal bone on each side of your head, your vestibular system is like a miniature space station, constantly monitoring your position and movement. This system works 24/7, even when you're asleep, sending crucial information to your brain about:
The Utricle: Your Internal Level
Imagine a carpenter's level, but microscopic and inside your ear. The utricle is a small, gravity-sensitive chamber that contains thousands of tiny calcium carbonate crystals called otoconia (literally "ear stones"). These crystals are normally embedded in a gel-like membrane, creating a natural level that helps your brain understand:
The Semicircular Canals: Your Motion Detectors
You have three fluid-filled canals in each ear, arranged like a three-dimensional gyroscope:
Each canal is filled with a fluid called endolymph and contains a motion sensor called the cupula – think of it as a tiny sail that bends when fluid moves past it.
The Problem Begins: For reasons that aren't always clear, some of your otoconia crystals break free from their normal location in the utricle. This can happen due to:
The Journey: These loose crystals then travel into one of your semicircular canals. The posterior canal is the most common destination (about 85% of cases) because of its position – gravity naturally pulls the crystals downward into this canal.
The Disruption: Once inside a semicircular canal, these crystals create chaos. Here's why:
Under normal circumstances, when you move your head, the fluid in your canals moves smoothly, bending the cupula and sending accurate signals about your movement to your brain.
With loose crystals present, they act like pebbles in a washing machine. When you change positions, these crystals tumble around, creating abnormal fluid movement that continues even after your head stops moving. This sends false, conflicting signals to your brain about movement that isn't actually happening.
Your brain relies on three main systems to maintain balance:
In BPPV, your affected inner ear sends incorrect movement signals while your eyes and body sensors report that you're still. This creates a sensory conflict that your brain interprets as spinning or movement – the hallmark of vertigo.
The Result: Your brain, trying to make sense of these conflicting signals, triggers:
The reason specific positions trigger your symptoms relates to how gravity affects the loose crystals:
Each movement creates a new pattern of abnormal fluid flow, triggering fresh episodes of vertigo.
While BPPV symptoms are intense, your brain has remarkable ability to adapt and compensate. Between episodes, most people function normally because their brain learns to rely more heavily on visual and body position cues. However, the definitive solution is to get those crystals back where they belong – which is exactly what BPPV treatments accomplish.
One of the most frustrating aspects of BPPV for many patients is not knowing why it happened to them. The truth is, while we understand exactly how BPPV works, the reason those crystals become loose in the first place often remains a mystery.
Idiopathic BPPV (meaning "of unknown origin") accounts for the majority of cases. If your doctor can't identify a specific trigger for your BPPV, you're in good company – this happens to most patients. Think of it like a shoelace that comes untied during the day; sometimes things just happen without a dramatic reason.
This doesn't mean something is wrong with you or that you did something to cause it. Your otoconia crystals may have simply reached a point where they became more fragile due to normal aging, or microscopic changes in your inner ear created the perfect conditions for them to break free.
Head Trauma: The Leading Known Cause
Head injuries are the most common identifiable cause of BPPV, particularly in people under 50. This doesn't necessarily mean severe trauma – even relatively minor incidents can dislodge crystals:
Studies show that about 18-20% of BPPV cases can be traced back to head trauma. The injury presumably shakes the crystals loose from their normal attachment, similar to how an earthquake might cause objects to fall from shelves.
Prolonged Bed Rest or Unusual Positioning
Extended periods lying in one position can sometimes trigger BPPV. This might happen after:
The theory is that staying in one position for too long may allow crystals to gradually shift out of their normal location.
Following Other Inner Ear Problems
BPPV sometimes develops after other inner ear conditions:
About 10-15% of BPPV cases follow these conditions. The inflammation may damage the structures that normally keep crystals in place, or the healing process may create conditions that make crystal displacement more likely.
Age: The Biggest Risk Factor
BPPV can occur at any age (documented cases range from 11 to 84 years old), but your risk increases significantly as you get older:
This age-related increase explains why BPPV often appears for the first time in middle age, even in people who've never had balance problems before.
Gender: Women Are Affected More Often
Women develop BPPV 2-3 times more frequently than men. While the exact reason isn't fully understood, potential factors include:
Other Considerations
Migraine Connection: While people with migraines may experience vertigo as part of their migraine symptoms, the relationship between migraine and BPPV specifically is still being studied. Some research suggests a possible connection, but migraine-related vertigo often behaves differently from typical BPPV.
Activity Level: Contrary to what you might expect, being sedentary doesn't appear to be a general risk factor for BPPV. The "prolonged positioning" trigger refers to specific situations of extended time in unusual positions, not overall activity level.
Unfortunately, since most BPPV cases are idiopathic, there's no reliable way to prevent first-time episodes. However, you can:
Whether your BPPV has an identifiable cause or not, it's crucial to understand that this condition isn't something you brought upon yourself. BPPV is a mechanical problem with a straightforward solution. Your crystals simply need to be guided back to where they belong, and with proper treatment, most people achieve excellent results.
Recover faster, move better, and feel stronger with expert physiotherapy. Our team is here to guide you every step of the way.

Here's some encouraging news: BPPV is one of the most successfully treatable causes of dizziness. Physiotherapy isn't just helpful for BPPV – it's the gold standard, first-line treatment with success rates consistently above 80-90% after just 1-3 treatment sessions.
The beauty of BPPV treatment lies in its elegant simplicity. Think of it like this: if marbles rolled into the wrong tube in a complex maze, you'd carefully tilt the maze until gravity helps them roll back to where they belong. That's essentially what physiotherapy does for your displaced ear crystals.
Repositioning maneuvers use precise head and body movements, combined with gravity, to guide those wayward crystals out of your semicircular canals and back into the utricle where they belong. Once back in their proper location, they reattach to the membrane and stop causing those disruptive signals that create vertigo.
For Posterior Canal BPPV (85% of cases)
The Epley Maneuver: The Gold Standard
Also called the Canalith Repositioning Procedure, this is the most widely used and researched treatment:
The Semont Maneuver: The Alternative Champion
This involves a swift 180-degree "cartwheel" motion from one side to the other:
For Horizontal Canal BPPV (10-15% of cases)
The BBQ Roll (Lempert) Maneuver
Named for its resemblance to turning food on a barbecue:
The Gufoni Maneuver
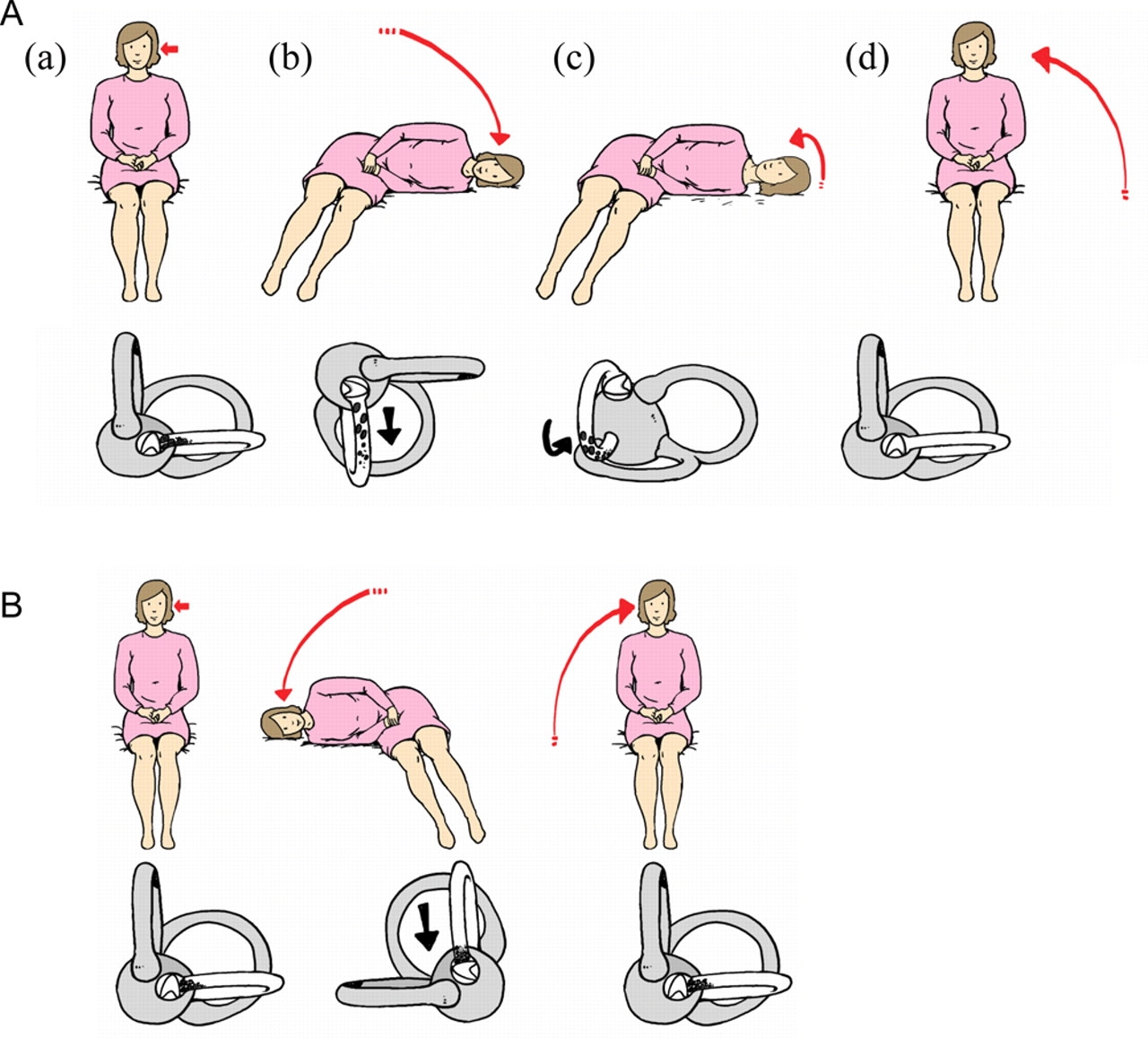
A newer technique that's particularly effective for certain subtypes:
For Anterior Canal BPPV (1.5-5% of cases)
Deep Head Hanging Maneuver
Since anterior canal BPPV is rare, this specialized technique is used when needed:
Brandt-Daroff Exercises: The Home Helper
These exercises serve multiple purposes:
Cawthorne-Cooksey Exercises: The Complete Package
These comprehensive exercises address multiple aspects of recovery:
General Vestibular Rehabilitation: The Confidence Builder
This broader approach focuses on:
Immediate Results
Many patients experience dramatic improvement right after their first treatment session. Don't be surprised if:
The Numbers That Matter
Research consistently shows:
When Multiple Sessions Are Needed
Some patients require 2-4 sessions for complete resolution. This might happen if:
Learning Self-Maneuvers
Your physiotherapist can teach you modified versions of repositioning maneuvers:
Understanding Recurrence
BPPV can return, with annual recurrence rates around 15%:
Compared to "Wait and See"
While BPPV sometimes resolves on its own, physiotherapy:
Compared to Medications
The bottom line: Physiotherapy for BPPV isn't just effective – it's remarkably so. Most patients achieve excellent results quickly, safely, and permanently.

Understanding your treatment plan helps reduce anxiety and sets realistic expectations. BPPV physiotherapy follows a proven, structured approach that's been refined through decades of research and clinical experience. Here's your roadmap to recovery.
The Detective Work: Identifying Your Specific Type of BPPV
Before treatment can begin, your physiotherapist needs to determine exactly which canal contains the displaced crystals. This isn't guesswork – specific tests reveal precisely what's happening in your inner ear.
The Dix-Hallpike Test: The Gold Standard for Posterior Canal BPPV
This might feel dramatic, but it's completely safe and highly informative:
The Roll Test: For Horizontal Canal BPPV
If your symptoms occur mainly when rolling over in bed:
Immediate Treatment: Getting Those Crystals Moving
Once your specific type of BPPV is identified, treatment begins immediately. Each maneuver is held for at least 30 seconds or until any vertigo and nystagmus subside.
For Posterior Canal BPPV (85% of cases): The Epley Maneuver
This four-step process might feel intense, but remember – the vertigo you experience means it's working:
Success rates you can count on: 80% success after one session, 92% with repeat treatments if needed.
For Horizontal Canal BPPV: The BBQ Roll
This technique "rolls" the crystals around the horizontal canal:
Alternative Techniques When Needed
What to Expect During Treatment
Post-Treatment Guidelines
The 24-Hour Rule: You may be advised to keep your head upright for 24 hours after treatment. This means:
Why these restrictions: They help ensure the crystals settle securely in their proper location.
Even after successful repositioning, your balance system needs time to readjust. This phase ensures lasting recovery and prepares you for independence.
Gaze Stabilization: Retraining Your Visual System
Your brain needs to relearn how to coordinate eye and head movements:
VOR (Vestibulo-Ocular Reflex) Exercises:
Cawthorne-Cooksey Exercises: The Complete Retraining Program
These time-tested exercises address multiple aspects of recovery:
Eye movement training:
Head movement exercises:
Balance challenges:
Patient Education: Your Toolkit for Success
Learning Self-Treatment
Your physiotherapist will teach you modified repositioning techniques:
Fall Prevention Strategies
BPPV increases fall risk, so you'll learn:
Activity Modification (Temporary)
Early in recovery, you'll learn:
Most patients don't need this phase, but it's invaluable for those with persistent symptoms or complex cases.
Who Benefits from Advanced Rehabilitation
Dynamic Balance Training: Real-World Preparation
Progressive challenges:
Advanced Cawthorne-Cooksey progression:
Dual-Task Training: Preparing for Daily Life
Real life requires doing multiple things simultaneously:
Functional Conditioning: Building Confidence
Comprehensive balance rehabilitation:
Week 1: Most patients experience significant improvement after 1-3 treatment sessionsWeek 2: Fine-tuning balance and movement confidenceWeeks 3-4: Advanced rehabilitation if needed, return to all normal activitiesOngoing: Occasional maintenance and recurrence management as needed
The Reality: BPPV can return in about 15% of patients annuallyThe Good News: Recurrence doesn't mean treatment failureYour Advantage: You'll have the tools and knowledge to manage it effectively
Why Recurrence Happens:
Your Response Plan:
This structured approach ensures not just symptom resolution, but also confidence, independence, and the ability to maintain your recovery long-term.

After years of treating BPPV patients, certain questions come up repeatedly. Here are detailed, honest answers to help you understand your condition and feel confident in your recovery journey.
This is one of the most common concerns, and it's completely understandable. There are several reasons why symptoms might return, and most are manageable:
BPPV Can Naturally Recur
The reality is that BPPV can come back. Research shows:
Incomplete Initial Resolution
Sometimes the first treatment doesn't move all the crystals:
Your Balance System Is Still Adapting
Even after successful repositioning, your balance system needs time to recalibrate:
Avoidance Can Actually Prolong Symptoms
Ironically, being too careful can work against you:
When to Seek Reassessment
Contact your physiotherapist if:
This is often the first question patients ask, especially during their first episode. The short answer is no, but let's explore what "benign" really means:
The Medical Definition of "Benign"
However, BPPV Can Still Be Significantly Disabling
While not dangerous to your overall health, BPPV can seriously impact your life:
Physical Impact:
Emotional and Social Impact:
The Reassuring Truth
This is a nuanced question that depends on several factors. Here's what you need to know:
Yes, But Only After Professional Diagnosis
Self-treatment can be highly effective, but only if you know exactly what type of BPPV you have:
Why Professional Diagnosis Matters:
Self-Treatment Success Rates (When Done Correctly)
The numbers are encouraging:
When Home Treatment Makes Sense
Ideal candidates for self-treatment:
Home Exercise Options
Self-administered Epley: Best for confirmed posterior canal BPPV recurrence
Brandt-Daroff Exercises: Good for general symptom management
When to Avoid Home Treatment
The Balanced Approach
Best practice combination:
Most BPPV patients don't need MRI, CT scans, or other imaging. However, certain situations warrant further investigation:
Standard BPPV Usually Doesn't Require Imaging
If you have typical BPPV that responds well to treatment:
Red Flags That Warrant Further Investigation
Contact your healthcare provider and consider imaging if you experience:
Neurological Warning Signs:
Atypical BPPV Patterns:
Treatment-Resistant Cases:
Specific Imaging Considerations
When your doctor might recommend imaging:
The Bottom Line on Imaging
Remember, the goal is always to get you the right treatment as efficiently as possible while ensuring nothing serious is missed.
Serving Vaughan, Thornhill, and Toronto. Direct billing available to most insurance providers.
✅ Canal-Specific Repositioning Expertise – Precise diagnosis and treatment for all types of BPPV
✅ 1-on-1 Physiotherapy with Vestibular Specialists – Dedicated, experienced practitioners
✅ High Success Rates with Just 1-2 Visits – Get back to your normal life quickly
📞 Call Now: 905-669-1221
📍 Clinic Address: 398 Steeles Ave W #201, Thornhill, ON L4J 6X3
🌐 Online Booking: www.vaughanphysiotherapy.com
Evening and weekend appointments available. Proudly serving Thornhill, Richmond Hill, Markham, Vaughan, and North York communities.
Explore the latest articles written by our clinicians