
Physiotherapy for chronic pelvic pain to improve mobility and reduce discomfort.
Chronic pelvic pain (CPP) is defined as cyclic or non-cyclic pain in the lower abdomen or pelvis lasting for at least six months. This requirement may be waived if central sensitization pain mechanisms are documented. It is a complex syndrome rather than a single disease, arising from interactions between the neurologic, musculoskeletal, and endocrine systems, and is further influenced by behavioral and psychological factors.
Common Symptoms
Prevalence
CPP is a major cause of morbidity and disability worldwide.
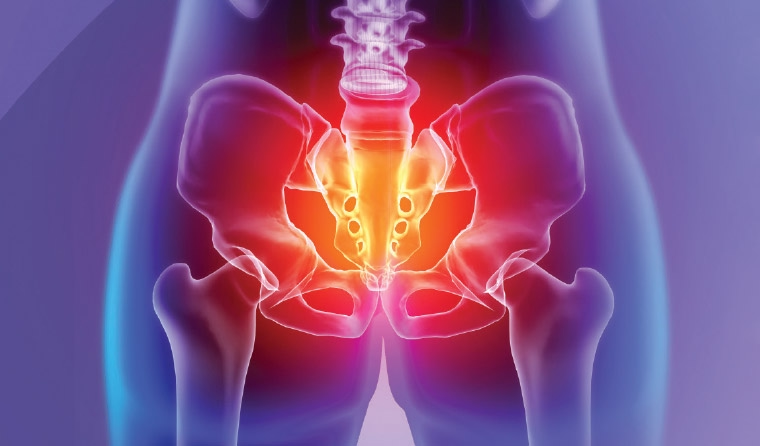
The pelvis is a complex structure made up of bones, muscles, nerves, and organs that work together to support movement and bodily functions.
Key anatomical components include:
Dysfunction in any of these structures can contribute to chronic pelvic pain.
Chronic pelvic pain (CPP) is defined as constant or intermittent pain in the lower abdomen or pelvis lasting for at least six months. It is not a single disease but a complex syndrome resulting from interactions between the neurologic, musculoskeletal, and endocrine systems.
Mechanisms of Development
The development of CPP often involves changes in how the central nervous system (CNS) processes pain signals:
Key Causes and Contributing Factors
The origin of CPP is not gynecologic in 80% of patients. The condition is typically multi-systemic:
Risk Factors and Biopsychosocial Influences
Physiotherapy is an indispensable component of recovery for chronic pelvic pain (CPP) because musculoskeletal pain and dysfunction are present in 50% to 90% of patients. As a complex syndrome rather than a single disease, CPP arises from the intricate interplay of the neurologic, musculoskeletal, and endocrine systems. Consequently, an integrated multidisciplinary approach involving a physiotherapist is essential for successful management.
Addressing Pelvic Floor Muscle Tension and Coordination
A primary focus of physiotherapy is managing pelvic floor muscle hypertonicity or spasms, which are a hallmark of conditions like levator syndrome.
Restoring Movement Patterns and Stability
Chronic pain frequently leads to physical compensations that further aggravate the condition.
Reducing Pain and Improving Daily Function
Physiotherapy targets both the primary pain and the functional limitations that diminish quality of life.
By integrating these techniques within a multimodal treatment plan, physiotherapy helps break the cycle of persistent pain and functional disability.
Recovery from chronic pelvic pain (CPP) is defined as a long-term process rather than an immediate fix, as the condition is a complex syndrome resulting from interactions between the neurologic, musculoskeletal, and endocrine systems. Because the origin of CPP is not gynecologic in 80% of patients, a multidisciplinary and multimodal approach tailored to the individual is essential for a positive prognosis.
Early Phase: Education and Initial Management
Intermediate Phase: Monitoring and Adjustment
Long-Term Phase: Maintenance and Expectations
Ultimately, recovery requires addressing the fact that organ-specific treatments often fail to alleviate CPP if central sensitization and myofascial dysfunction are left untreated. Success is best achieved when the interdisciplinary team addresses all biopsychosocial factors, including sleep, mood, and environmental stress, alongside physical treatments.
Recover faster, move better, and feel stronger with expert physiotherapy. Our team is here to guide you every step of the way.

Physiotherapy is an essential component of recovery for chronic pelvic pain (CPP) because musculoskeletal pain and dysfunction are present in 50% to 90% of patients. Clinical guidelines emphasize that focusing exclusively on visceral or organic causes while neglecting myofascial dysfunction can lead to prolonged pain and unnecessary surgical interventions.
Pelvic Floor Muscle and Manual Therapy
These techniques specifically target myofascial trigger points, which are localized areas of deep muscle tenderness within a tight band of muscle in the abdominal wall or pelvic floor.
Breathing and Relaxation Techniques
A major objective of physiotherapy is to restore the patient's ability to voluntarily relax the pelvic floor muscles, which are often in a state of hypertonicity or spasm. These techniques are most effective when combined with pain education, which helps patients understand how the central nervous system modulates their pain experience and manages expectations for long-term care.
Postural Correction and Movement Retraining
Physiotherapists identify and correct mechanical issues that can generate or exacerbate pain. Women with CPP often present with uneven gait, discrepancies in limb length, restricted range of motion, and postural asymmetry, such as leaning to one side to avoid pain. Addressing these biomechanical factors is critical, as musculoskeletal dysfunction is often a primary generator of the pain syndrome.
Core Stabilization and Exercise
Targeted exercise programs are essential for patients to regain pelvic stability, particularly those suffering from pelvic girdle pain. Moderate, regular exercise is recommended as a vital component of a multimodal treatment plan for various chronic pain conditions, including fibromyalgia and chronic low back pain.
Adjuvant Therapeutic Tools
Physiotherapists may use specialized tools to enhance tissue elasticity and functional tolerance:
CPP is defined as cyclic or non-cyclic pain lasting at least six months. It is not a single disease but a complex syndrome involving interactions between the neurologic, musculoskeletal, and endocrine systems, often self-perpetuated by central sensitization.
Why These Prevention Strategies Are Effective
Integrated Management and the Path to Recovery
Sources strongly support the necessity of a multidisciplinary approach for long-term management.
Success in managing CPP often requires a shift from seeking a "cure" for a single organ to a biopsychosocial model that addresses sleep, mood, and movement together.
This specialized approach to rehabilitation for chronic pelvic pain (CPP) is highly consistent with current clinical consensus guidelines, which define the condition as a complex syndrome rather than a single disease,. Because CPP results from the interaction between neurologic, musculoskeletal, and endocrine systems, an integrated multidisciplinary approach is essential for long-term success,.
The Foundation: Comprehensive Assessment
A thorough assessment is critical because 80% of CPP cases are not gynecologic in origin,.
Therapeutic Interventions and Education
Progression and Monitoring
Recovery from CPP is a long-term process requiring shared decision-making and the setting of functional goals rather than just pain reduction,.
By targeting the actual drivers of persistent pain—the central nervous system and the musculoskeletal system—rather than focusing solely on visceral structures, this integrated approach addresses the multi-systemic nature of chronic pelvic pain,.
Do I need a referral for pelvic physiotherapy?
Don't let chronic pelvic pain limit your activities or affect your daily life. Our experienced team is ready to help you build a strong foundation for lasting recovery.
Book Your Specialized Assessment Today:
Phone: 905-669-1221
Location: 398 Steeles Ave W #201, Thornhill, ON L4J 6X3
Online Booking: www.vaughanphysiotherapy.com
Serving communities across Thornhill, Langstaff, Newtonbrook, Willowdale, North York, Markham, Richmond Hill, Concord, and North Toronto.
Conveniently located in the heart of Thornhill, offering flexible scheduling to accommodate your recovery needs.
Created by Sara Lam
Explore the latest articles written by our clinicians