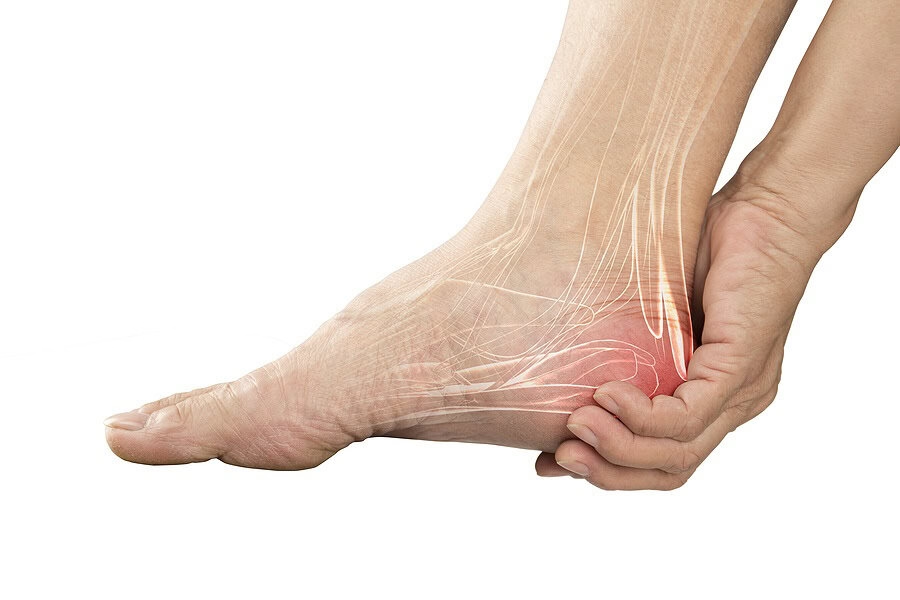
Stress fracture of the long bones in the foot.
A metatarsal stress fracture is defined as the spontaneous fracture of normal bone that results from the summation of stresses, where any single stress event would ordinarily be harmless. These injuries are most commonly caused by the repetitive overloading of a particular metatarsal. Stress fractures are thought to result from alternating compressive and tensile forces transmitted to the bone via ligaments, tendons, and muscles.
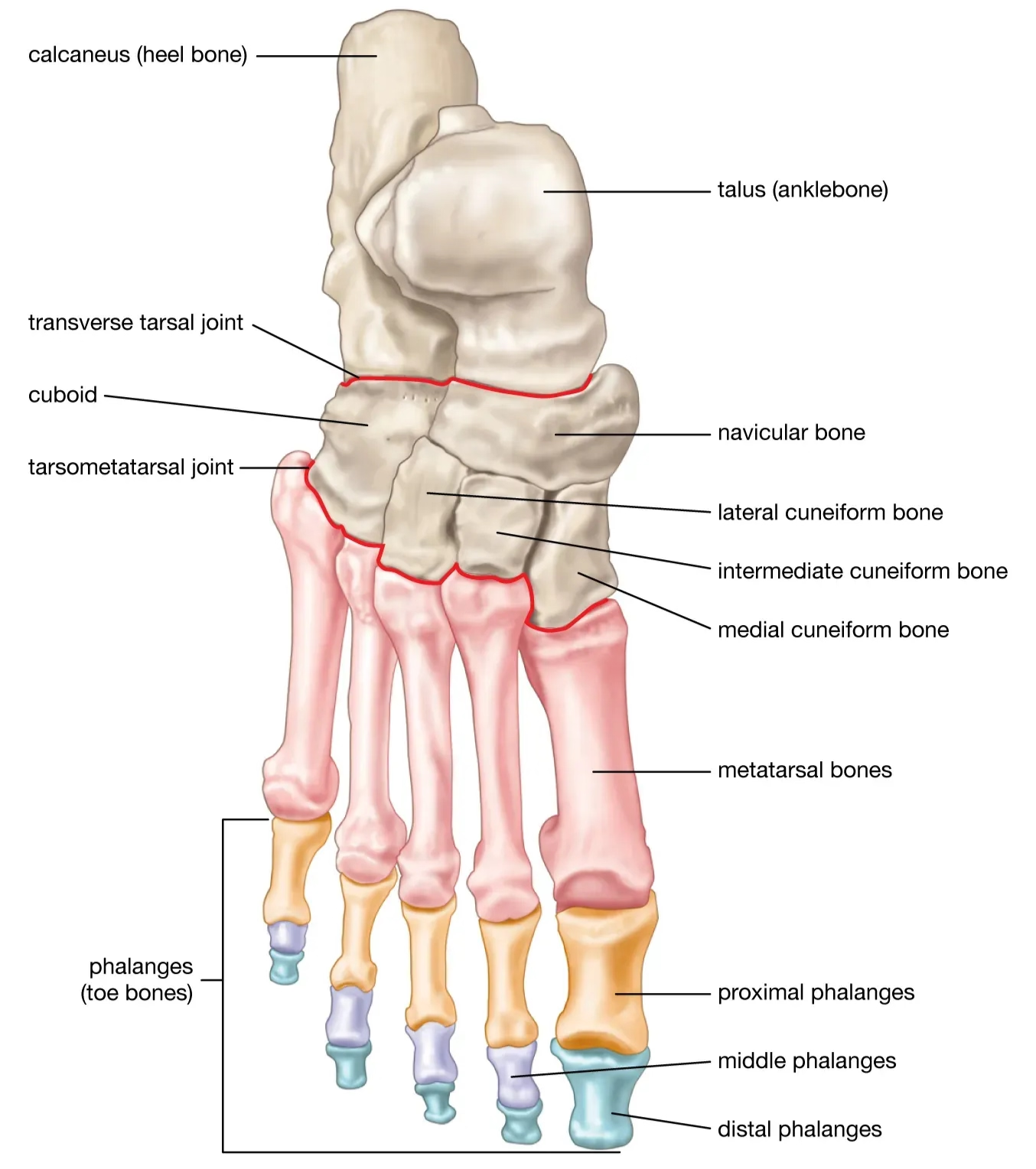
Patients sustaining metatarsal stress fractures typically present with an insidious onset of pain in the forefoot. Key symptoms include:
Diagnosis relies heavily on a careful history and physical examination, as initial radiographs may not reveal the fracture until 3 to 6 weeks after the onset of symptoms, when cortical hypertrophy or fracture lines become apparent.
Stress fractures of the metatarsals are generally concentrated in the middle metatarsals, specifically the second and third metatarsal shafts. These two locations account for a high concentration of metatarsal fractures (39% in the second and 41% in the third). Overall, stress fractures of the second, third, and fourth metatarsals collectively account for 90% of metatarsal injuries.
The high incidence in the second metatarsal is supported by mechanical analysis showing that the bending strain (6.9 times greater than the first metatarsal strain) and shear force are greatest in the second metatarsal shaft during running.
Metatarsal stress fractures are frequently encountered in specific populations:
Common contributors also include:

Recover faster, move better, and feel stronger with expert physiotherapy. Our team is here to guide you every step of the way.

Physiotherapy helps guide safe healing, reduce pain, and correct the underlying mechanical factors that caused the fracture. Treatment focuses on:
A structured rehab plan ensures the bone heals fully before returning to impact activities.
The length of recovery depends on the severity of the stress fracture and adherence to offloading:
Early phases focus on rest and protection; later phases gradually reintroduce walking, strengthening, and eventually running.
Your rehabilitation program will be tailored to your activity level and the severity of injury. Treatment may include:
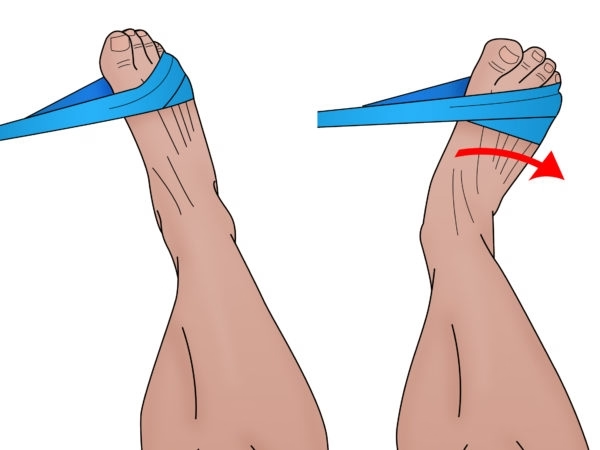
Preventing recurrence requires addressing both strength and mechanics. Your physiotherapist will guide you through:
A long-term conditioning plan helps keep your feet resilient and reduces the likelihood of future bone stress injuries.
Can I walk on a metatarsal stress fracture?
You can, but too much walking slows healing and can worsen the crack. Keep steps low, avoid long walks, and use a stiff shoe or boot if advised.
Do I need a boot?
You need a boot if walking is painful, swelling is noticeable, or imaging confirms a fracture. Early stress reactions may not require one.
How long does it take to heal?
Most cases heal in 6–10 weeks.
More advanced or repeated fractures can take 12+ weeks, especially if you continue overloading the foot.
When can I run again?
Only once you can walk pain-free.
For most people, this happens around 6–10 weeks. Running too early almost always delays healing.
Should I use ice?
Yes, ice is important, especially in the early stage.
Ice helps reduce pain and swelling around the injured area.
Use for 10–15 minutes at a time, a few times per day.
What happens if I ignore the pain?
The stress fracture can deepen, become a full fracture, or turn into a chronic injury. Ignoring it significantly lengthens recovery and may lead to long-term pain.
How do I prevent it from coming back?
Address the root causes:
These are the key ways to reduce recurrence.
Don’t let foot pain or a metatarsal stress fracture limit your daily movement, training, or lifestyle. Our experienced team at Vaughan Physiotherapy Clinic has helped countless patients recover safely, rebuild strength, and return to activity with confidence.
Book Your Specialized Assessment Today:
Serving Thornhill, Langstaff, Willowdale, North York, Markham, Richmond Hill, and surrounding communities. Evening/weekend appointments available.
Explore the latest articles written by our clinicians