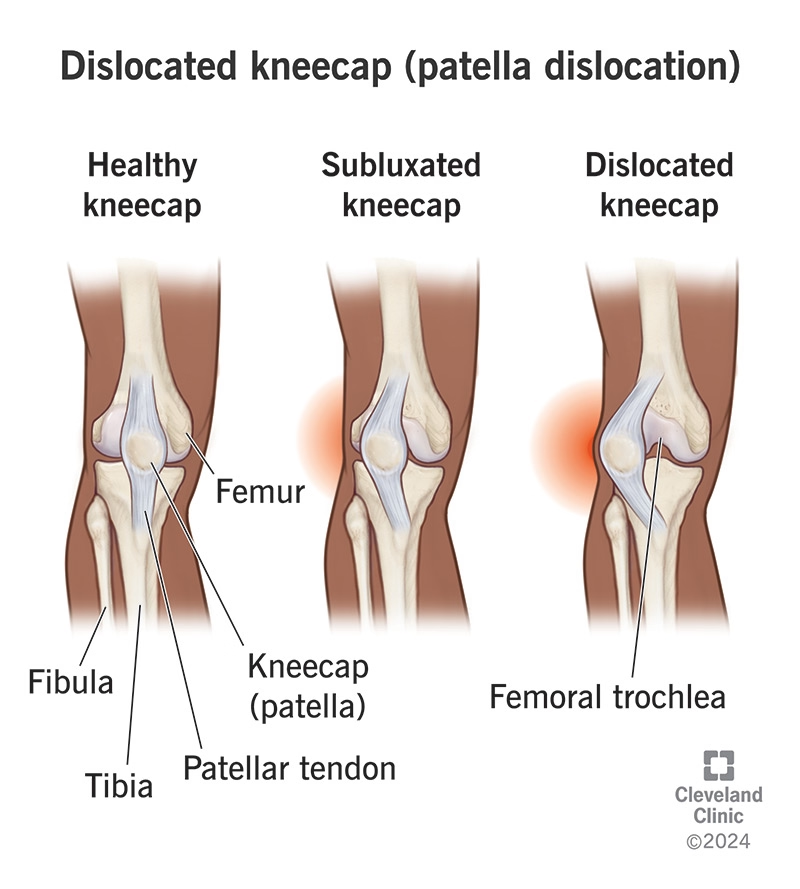
Why Physiotherapy is Essential for Patellar Subluxation/Dislocations
Physiotherapy is considered the cornerstone treatment in managing patellar instability, as it aims to restore function and reduce recurrent instability by improving modifiable impairments like knee joint movement, lower limb muscle strength, and dynamic control.
Strengthening Quadriceps and Hip Muscles for Stability
Restoring strength in the lower limb is a primary focus of rehabilitation because these muscles control the motion and loads applied to the hip and knee.
- Quadriceps and VMO: Strengthening the quadriceps, specifically the vastus medialis oblique (VMO), is essential to counteract the stronger lateral tissues that can pull the kneecap out of alignment. Because local pain and swelling from the injury can reduce quadriceps activation, early management is critical to prevent muscle atrophy.
- Hip and Core Muscles: Exercises targeting the gluteal and core muscles are increasingly recommended. Strengthening the hip abductors (like the gluteus medius) and extensors helps stabilize the entire kinetic chain, reducing the mechanical stress on the patellofemoral joint.
Retraining Patellar Tracking During Movement
Patients with instability often exhibit abnormal patellar tracking over the femoral groove during motion.
- Movement Strategies: Physiotherapy interventions include exercises that aim to retrain functional movement strategies. This involves modifying trunk and lower limb alignment to reduce the lateral orientation of the quadriceps force, which essentially protects the kneecap from slipping outward.
- Dynamic Medial Stability: Some specialized approaches include adductor strengthening (e.g., ball squeezes), as these muscles are anatomically connected to the VMO and can help improve the dynamic medial stability of the patella.
Improving Balance and Proprioception to Prevent Recurrence
Proprioception—the body's ability to sense its position in space—often deteriorates significantly following a patellar dislocation.
- Neuromuscular Control: Physiotherapy uses neuromuscular and balance exercises (such as single-leg stands or wobble board activities) to retrain the proprioceptive neurological system.
- Reducing Re-injury Risk: Improving this "dynamic control" is vital for preventing re-injury during high-demand activities where the kneecap is most vulnerable, such as single-leg landings.
Guiding a Safe Return to Sport
A structured, phased progression is critical for athletes to return to sports safely and avoid the high risk of recurrence.
- Staged Progression: Rehabilitation typically progresses through distinct stages: from static strengthening to dynamic proprioception, followed by running, and eventually plyometrics (e.g., box jumps).
- Sport-Specific Drills: Before full return, therapists guide patients through sport-specific tasks like cutting, pivoting, and jumping to ensure they can control landings without the knee collapsing into a "valgus" (knock-knee) position.
- Psychological Readiness: Beyond physical strength, comprehensive rehabilitation addresses a patient's psychological readiness and understanding of their specific tasks to ensure a successful return to daily life and sport.
Furthermore, maintaining long-term muscle strength through physiotherapy may help maintain long-term knee health, as strong quadriceps are associated with less cartilage loss in patients at risk for patellofemoral osteoarthritis
What to Expect: Prognosis and Recovery Timeline
First-Time Dislocation: 6–12 Weeks of Rehabilitation
A national survey of physiotherapists in the UK found that the most common treatment duration for a first-time dislocation ranges from 7 weeks to 3 months.
- Initial Phase: Treatment often begins with a period of immobilization (3–4 weeks) in an extension splint or brace to manage acute pain and swelling.
- Exercise Duration: Experts recommend that patients perform prescribed exercises for at least 3 months to achieve the necessary neuromuscular adaptations to resistance training.
- Self-Management: Some studies are investigating whether a single session of expert advice and a structured home program is as effective as multiple supervised sessions for these patients.
Recurrent Instability: 3–6 Months of Structured Rehab
For patients with recurrent instability or those who do not respond to initial care, a more intensive approach is required.
- Supervised Rehabilitation: Structured programs, such as those in the PRePPeD trial, typically involve four to six one-to-one sessions over a maximum of 6 months.
- Surgical Consideration: If conservative options are exhausted and a patient remains symptomatic with recurrent dislocations, surgical intervention is indicated. Patients with recurrent instability have a six times greater risk of persistent instability if treated with active rehabilitation alone compared to those who combine rehabilitation with surgery.
Post-Surgical Stabilization (MPFL Reconstruction): 4–9 Month Timeline
Following a Medial Patellofemoral Ligament (MPFL) reconstruction, recovery follows a staged progression to ensure the graft matures while restoring full function.
- Early Recovery (Weeks 1–10): Focuses on restoring range of motion, achieving full weight-bearing, and starting advanced strengthening exercises.
- Return to Impact (4–5 Months): Jogging and mild sports activity typically begin around 4 months (10–21 weeks), followed by plyometrics (box jumps and hopping) between 13 and 23 weeks.
- Full Return to Sport: While some sources suggest a full return at 6 months, a case series of seven subjects showed that the actual return to sport or full functional activity occurred between 19 and 36 weeks (roughly 4.5 to 9 months).
Factors Influencing Prognosis
- Recurrence Risk: Approximately one in four people who suffer a first-time dislocation will experience another within ten years.
- Functional Outcomes: While surgery is associated with a lower rate of re-dislocation, it is currently unclear if it results in significantly better functional outcomes compared to high-quality conservative management.
- Long-Term Health: Successful rehabilitation is critical because patellar dislocation increases the long-term risk of developing patellofemoral osteoarthritis
Physiotherapy Treatment Approaches
The physiotherapy treatment approaches for patellar instability are designed to address the "multi-factorial" nature of the condition, focusing on correcting muscle imbalances, restoring dynamic control, and managing acute injury responses like pain and swelling. While practice varies, evidence-based programs generally follow a phased progression from initial protection to high-level functional loading.
Phase 1: Acute Management (0–2 weeks)
The primary goal is to manage the acute response—local pain, swelling, and inflammation—which can inhibit quadriceps activation and lead to muscle atrophy.
- RICE and Protection: Initial management often involves the PRICE protocol (Protection, Rest, Ice, Compression, Elevation) to minimize secondary injury.
- Bracing and Taping: Clinicians frequently use a patella-stabilizing brace or peripatellar taping for the first three weeks to provide stability while allowing controlled movement. Taping has been shown to result in better functional outcomes and less muscle atrophy compared to rigid cylinder casts.
- Early Range of Motion (ROM): Exercises often start with active (AROM) or active-assisted knee flexion in sitting or long sitting to prevent joint stiffness and adhesions.
- Isometric Activation: Early quads engagement is critical. This includes static quadriceps contractions (quad sets) and straight leg raises (SLR) to provide a superior glide of the patella and promote engagement in the trochlear groove.
Phase 2: Strength & Control (2–6 weeks)
Once acute symptoms subside, the focus shifts to restoring muscle capacity and joint control.
- VMO and Adductor Recruitment: While specific vastus medialis oblique (VMO) strengthening is common, the sources suggest that adductor strengthening (e.g., hook-lying ball squeezes) is highly effective because the MPFL is anatomically connected to the adductors. Firing the adductors can help recruit the VMO for improved dynamic medial stability.
- Hip and Gluteal Strengthening: Strengthening the hip abductors (gluteus medius) and extensors is essential for controlling lower-limb loads. This helps stabilize the kinetic chain and reduces the lateral orientation of the quadriceps force.
- Balance Training: Static proprioception exercises, such as single-leg stands or weight shifting, are initiated to retrain the proprioceptive neurological system that is often impaired after dislocation.
Phase 3: Functional & Sport-Specific (6–12 weeks)
This phase bridges the gap between basic strength and high-demand activities.
- Dynamic Loading: Exercises progress to closed kinetic chain movements like step-ups, lunges, and resisted squats. Physiotherapists often use objective strength assessments (like hand-held dynamometry) to ensure symmetry between limbs.
- Movement Retraining: A key focus is modifying trunk and lower-limb alignment to reduce "shear forces". During plyometric drills (e.g., box jumps or hopping), subjects are trained to land without trunk lean, hip drop, or genu valgus (knock-knee position).
- Running Progression: Interval training and modifications in stride length or cadence are introduced based on the patient's endurance and functional goals.
Phase 4: Return-to-Play (3–6 months)
The final stage involves a gradual reintegration into full sporting demands.
- Sport-Specific Agility: Drills include cutting, pivoting, and deceleration maneuvers tailored to the patient’s specific sport (e.g., soccer, track, or cross-training).
- Clearance and Readiness: Beyond physical strength, the sources emphasize the importance of psychological readiness and a comprehensive understanding of the athlete's tasks. Successful return is often defined by the absence of residual pain and no early re-injury
Prevention & Long-Term Management
Maintain Quadriceps, VMO, and Glute Strength
Consistent strengthening is the most critical factor for long-term knee health. Because the physiological adaptations to exercise are reversible once training stops, experts recommend performing strengthening exercises at least one to two times per week to maintain muscle mass and protective function.
- Quadriceps and VMO: Stronger quadriceps are not only vital for patellar stability but are also associated with reduced cartilage loss and better long-term outcomes regarding patellofemoral osteoarthritis.
- Gluteal Muscles: Strengthening the gluteus medius and hip abductors is essential for controlling the loads applied to the knee and maintaining proper alignment during dynamic movements.
Taping and Bracing for High-Risk Activities
For individuals with a history of instability, external supports can provide an additional layer of protection during high-demand tasks:
- Bracing: While the use of a stabilizing brace is standard during the first few weeks of recovery to prevent muscle atrophy, specialized patellar braces or bandages are often recommended for ongoing protection in sports.
- Taping: Physiotherapists may utilize various taping techniques to assist with patellar tracking or to provide "unloading" support for athletes returning to high-risk environments.
Gradual Return and Clearance for High-Impact Sports
A sudden return to sports involving cutting or pivoting significantly increases the risk of re-injury, as approximately 61% of primary dislocations occur during sports activities.
- Phased Progression: Athletes should only return to full sport after successfully completing a progression of sport-specific drills, including deceleration, pivoting, and cutting maneuvers.
- Clinical Criteria: Clearance should be based on a comprehensive evaluation of quadriceps strength, joint laxity, and psychological readiness to ensure the patient can successfully handle the specific tasks of their sport.
Correction of Faulty Mechanics
Preventing recurrence involves retraining movement strategies to reduce the lateral forces that pull the kneecap out of its groove.
- Landing Control: During plyometric activities (like jumping or hopping), it is vital to demonstrate the ability to control the landing without allowing the knee to collapse into a genu valgus (knock-knee) position.
- Alignment Correction: Training focuses on modifying trunk lean and hip drop to ensure that forces are absorbed efficiently through the entire kinetic chain rather than being concentrated on the patellofemoral joint
FAQs
- Can a patellar dislocation heal without surgery
- Yes, most first-time, isolated acute patellar dislocations are managed non-surgically, especially in the absence of significant bone or cartilage damage. Physiotherapy is considered the "corner-stone" of this conservative approach, focusing on restoring knee movement, improving muscle strength, and regaining dynamic control. While many patients recover without permanent functional limitations using these methods, research indicates that approximately 40% of patients may continue to experience recurrent instability or symptoms following non-operative care.
- When is surgery necessary?
- Structural Damage: Surgery is indicated if the dislocation is associated with large displaced osteochondral fractures (greater than 5 mm), intraarticular loose bodies, or a complete avulsion of the vastus medialis oblique (VMO) muscle.
- Recurrent Instability: If a patient experiences repeated dislocations and remains symptomatic after conservative options have been exhausted, surgical stabilization—most commonly Medial Patellofemoral Ligament (MPFL) reconstruction—is often the treatment of choice.
- Persistent Instability Risk: Patients with recurrent dislocations have been found to have a six times greater risk of persistent instability if treated with rehabilitation alone compared to those who combine rehabilitation with MPFL reconstruction.
- How soon can I return to sport?
- Non-Surgical Recovery: For most first-time dislocations treated with physiotherapy, the rehabilitation duration typically ranges from 7 weeks to 3 months. It is recommended that patients perform prescribed exercises for at least three months to allow for necessary neuromuscular adaptations.
- Surgical Recovery: The timeline for returning to sport following an MPFL reconstruction is significantly longer. While some initial sports activities like jogging may begin around 4 months (16 weeks), a full return to high-demand functional activity or sport generally requires between 19 and 36 weeks (roughly 4.5 to 9 months)
Our Specialized Approach to Patellar Instability Rehab
A specialized approach to rehabilitation for patellar instability focuses on correcting modifiable impairments—such as reduced lower limb muscle strength and poor dynamic control—to restore function and prevent recurrence. The following components describe the core pillars of this evidence-based strategy:
Targeted Quadriceps and VMO Strengthening
- Addressing Muscle Inhibition: Acute dislocations typically cause local pain and swelling, which can inhibit quadriceps activation and lead to significant muscle atrophy.
- Medial Stability: Rehabilitation prioritize the vastus medialis oblique (VMO) to counteract stronger lateral tissues that can pull the kneecap out of alignment. Specific exercises, such as isometric quadriceps sets and straight leg raises, are used to provide a superior glide of the patella and promote engagement in the femoral groove.
- Adductor Integration: Some protocols incorporate adductor strengthening (e.g., ball squeezes) because these muscles share an anatomical layer with the medial patellofemoral ligament (MPFL) and can help recruit the VMO for improved medial stability.
- Progressive Overload: Effective programs utilize evidence-based resistance guidelines, advising patients to increase loads once they can comfortably complete three sets of 12 repetitions.
Hip and Glute Retraining
- Load Control: Strengthening the hip and thigh muscles is essential because they play a primary role in controlling the motion and loads applied to both the hip and the knee joint.
- Gluteal Stability: Retraining the gluteus medius and other hip abductors is a "key factor" in preventing the lateral orientation of quadriceps forces that lead to instability.
- Kinetic Chain Balance: Core and gluteal strengthening are emphasized to stabilize the entire lower limb and minimize the evolution toward recurrent dislocations during high-demand movements.
Proprioceptive and Balance Drills
- Addressing Deficits: Patellar dislocations often result in a significant deterioration of proprioceptive capability.
- Movement Retraining: Drills aim to retrain movement strategies by modifying trunk and lower limb alignment (e.g., avoiding trunk lean or hip drop) to reduce the lateral pull on the patella during functional tasks.
- Staged Progression: Balance training moves from static drills, such as single-leg stands, to dynamic proprioception involving cone touches, wobble boards, or BOSU activities.
Return-to-Sport Testing and Progression
- Staged Recovery Timeline: Athletes follow a structured progression: Stage III involves running (weeks 10–21), Stage IV includes plyometrics like box jumps (weeks 13–23), and Stage V involves sport-specific drills such as cutting and pivoting (weeks 14–19).
- Objective Testing: Clearance for return to sport is guided by objective leg muscle strength assessments (often using hand-held dynamometry) and balance testing tailored to the specific demands of the athlete's sport.
- Comprehensive Readiness: Successful return requires more than physical strength; it includes clinical exams for laxity and an assessment of psychological readiness for the specific tasks of the sport.
- Final Outcomes: While some activities may resume earlier, a full return to high-demand sport or functional activity typically occurs between 19 and 36 weeks
Take the First Step Toward Recovery
Don't let subluxations and dislocations limit your activities or affect your daily life. Our experienced team is ready to help you build a strong foundation for lasting recovery.
Book Your Specialized Assessment Today:
Phone: 905-669-1221
Location: 398 Steeles Ave W #201, Thornhill, ON L4J 6X3
Online Booking: www.vaughanphysiotherapy.com
Serving communities across Thornhill, Langstaff, Newtonbrook, Willowdale, North York, Markham, Richmond Hill, Concord, and North Toronto.
Conveniently located in the heart of Thornhill, offering flexible scheduling to accommodate your recovery needs.
Created by Sara Lam