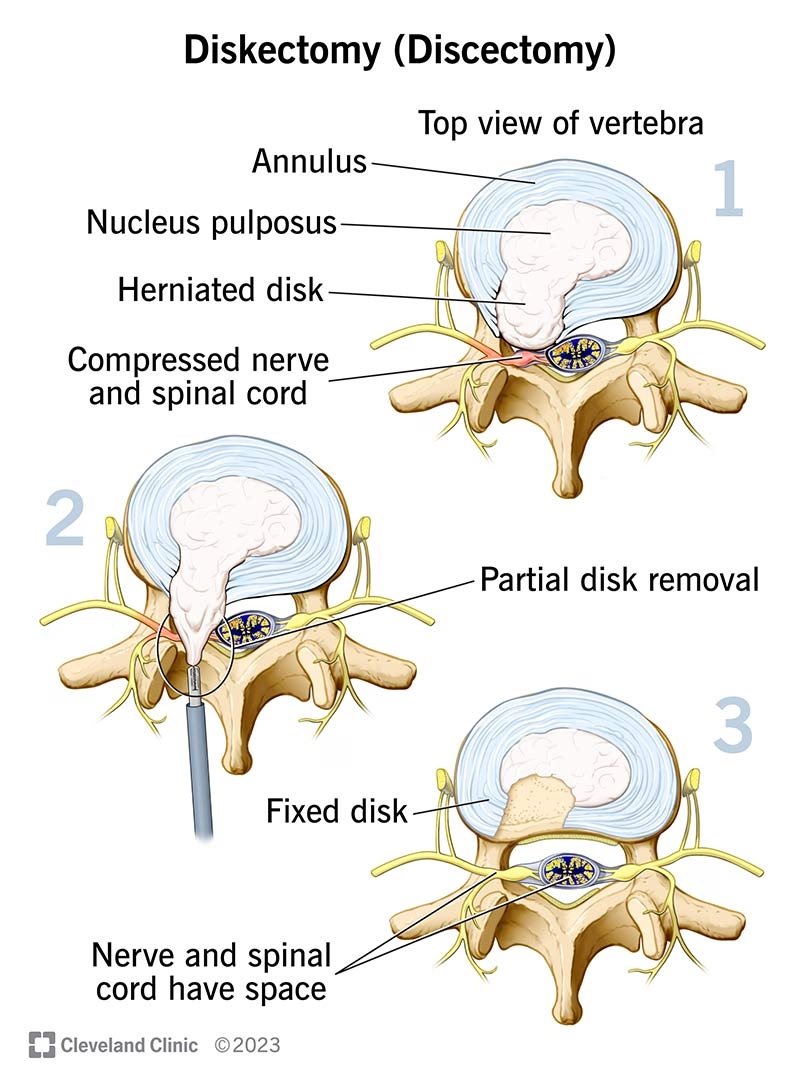
Why Physiotherapy Is Critical for Discectomy Recovery
Post-surgical physiotherapy is considered a vital supplement to lumbar discectomy because surgery alone may not address the muscular deconditioning and functional impairments that often persist or develop after the procedure. In fact, up to 40% of patients continue to experience residual pain, motor deficits, or decreased functional status following surgery.
Restoring Mobility and Function
- Improving Lumbar Mobility: Following disc excision, spinal mobility is typically restricted to approximately 60% of normal levels at the three-month mark. Specialized rehabilitation utilizes stretching, joint mobilization, and range-of-motion exercises to restore flexibility and prevent long-term spinal dysfunction.
- Restoring Functional Movement: Rehabilitation aims to correct a "distorted body schema" (an altered mental representation of the back) and modify motor control patterns to ensure a safe resumption of daily activities.
Targeting Core and Trunk Stability
- Re-activating Deep Core Stabilizers: The lumbar multifidus (LM) and transversus abdominis (TrA) are critical for spinal stability, yet they frequently exhibit atrophy, decreased activation, and fatty infiltration after surgery. Because recovery of these muscles is not automatic after pain resolves, motor control exercises are essential to re-train their activation.
- Increasing Strength and Endurance: High-intensity exercise programs that target the pelvic, hip, and trunk muscles have been shown to lead to a faster decrease in pain and disability than lower-intensity care.
Neural Recovery and Pain Management
- Reducing Residual Symptoms: Techniques like neural mobilization (e.g., nerve gliding) are used to maintain the "gliding" of spinal nerves, reduce local edema, and alleviate residual sciatica.
- Posture and Mechanics: Early education focuses on maintaining neutral lumbar lordosis and safe body mechanics (such as "log-rolling" out of bed) to protect healing tissues while they are most vulnerable.
What to Expect: Prognosis and Recovery Timeline
The prognosis for recovery after a lumbar discectomy is generally positive, with success rates typically ranging between 78% and 95% at one to two years post-operation. Sources provide evidence that supports your proposed recovery timeline, while adding specific clinical details regarding the intensity and focus of rehabilitation at each stage.
0–2 Weeks: Immediate Post-Operative Phase
The primary focus during this window is safety, education, and early mobilization.
- Education and Posture: Patients are instructed on maintaining a neutral lumbar lordosis and using safe strategies for activities of daily living, such as "log-rolling" to arise from bed.
- Early Mobility: In low-risk patients, lifting activity restrictions and returning to activity as early as two weeks post-surgery has been shown to shorten sick leave without increasing the risk of reherniation or complications.
- Immediate Activation: Some protocols initiate gentle exercises, such as knee and hip flexion, as early as two hours after surgery. Formal motor control exercises to re-train the transversus abdominis (TrA) and lumbar multifidus (LM) can be successfully initiated as early as 10 days post-operation.
2–6 Weeks: Early Rehabilitation Phase
During this phase, symptoms begin to stabilize, and formal exercise programs typically commence.
- Symptom Reduction: Most patients experience a significant reduction in leg pain (sciatica) and functional disability by the six-week mark.
- Initiation of Formal Training: While mobilization starts earlier, the most common window for beginning a structured therapeutic exercise program is 4 to 6 weeks post-surgery.
- Motor Control: Rehabilitation often begins with isolated volitional contractions of the deep core stabilizers (TrA and LM) in positions like quadruped or supine to restore spinal stability.
6–12 Weeks: Progressive Strengthening Phase
This period marks the transition to more intensive physical demands and global muscle strengthening.
- Intensive Strengthening: Formal "Early Active Training" programs often enter a second, more intensive phase at 6 weeks, focusing on intensive muscle strength, trunk extensors, and cardiovascular conditioning.
- Endurance and Power: Exercise approaches during this phase utilize sustained isometric contractions to increase the strength and endurance of global trunk muscles while minimizing potentially harmful shear loading of the spine.
- Return to Work: Research indicates that the median time for return to work is between 6 and 8 weeks. Patients in high-intensity exercise programs have been shown to return to work significantly faster (average of 56 days) compared to those in low-intensity care (75 days).
3–6 Months and Beyond: Long-Term Recovery
The final phase focuses on maintaining functional gains and establishing long-term health habits.
- Near-Full Recovery: While many feel significantly better, it is important to note that back muscle strength may actually decrease for the first three months post-operatively before showing significant improvement through rehabilitation.
- Return to High-Demand Activity: Long-term goals include a full return to work, sport, and heavy lifting. Some protocols include cardiovascular activities like swimming and jogging starting as early as the 12th week.
- Long-Term Adherence: Most structured programs last approximately 12 weeks. However, adherence to home exercise often drops significantly after the first two months, suggesting that a long-term, self-managed conditioning program is essential to preserve functional health for a decade or more
Physiotherapy Treatment Approaches
The physiotherapy treatment approaches following a lumbar discectomy transition from early protection and muscle re-education to high-intensity functional training. Evidence sources indicate that while individual protocols vary, structured rehabilitation starting four to six weeks post-surgery significantly accelerates the reduction of pain and disability.
1. Early Recovery Phase (0–6 Weeks)
Rehabilitation in this phase focuses on managing post-surgical symptoms and re-establishing basic motor control while protecting healing tissues.
- Pain and Swelling Management: Early exercises, such as knee and hip flexion initiated as early as two hours post-surgery, are used to reduce local edema and maintain neural mobility.
- Education on Posture: Patients receive instruction on maintaining a neutral lumbar lordosis and using safe strategies for daily tasks, such as "log-rolling" to arise from bed.
- Walking Program: Daily walking is encouraged immediately to improve circulation and mobility. A 12-week program focused on walking has been shown to increase oxygen consumption and training effects without increasing pain.
- Gentle Core Activation: Specific motor control exercises to re-educate volitional contractions of the transversus abdominis (TrA) and lumbar multifidus (LM) can be initiated as early as 10 days post-surgery.
- Neural Mobility: Passive and active exercises for neural mobilization (e.g., nerve gliding) may be used to reduce residual leg symptoms, though evidence suggests they may not provide significant additional benefits over standard care in the very short term.
2. Mobility and Strengthening Phase (6–12 Weeks)
As the surgical site stabilizes, the focus shifts toward restoring spinal flexibility and building foundational strength.
- Increasing Mobility: Treatment includes stretching and range-of-motion (ROM) exercises to restore lumbar and hip flexibility, which is often restricted to 60% of normal levels at three months post-excision.
- Progressing Core Stabilization: After approximately three weeks, exercises emphasize the endurance of deep stabilizers using sustained isometric contractions in positions like quadruped (arm/leg lifts) and horizontal side supports.
- Lower-Limb Strengthening: Programs incorporate strengthening for the pelvic, hip, and trunk muscles to provide global support for the spine.
- Gait and Endurance: Progressive walking or submaximal bicycle training is used to build cardiovascular endurance.
- Functional Patterns: Patients begin modifying motor control patterns to safely resume bending and lifting, often utilizing back school education to manage expectations and reduce fear.
3. Functional and Advanced Training
Advanced rehabilitation prepares the patient for high-demand activities through increased intensity and specificity.
- Intensive Strengthening: Evidence suggests that high-intensity exercise protocols lead to a faster decrease in pain and disability than low-intensity programs.
- Cardiovascular Conditioning: Protocols often introduce more demanding activities, such as swimming and jogging, starting around the 12th week.
- Work and Sport-Specific Training: Rehabilitation moves to functional weight-bearing and tasks specific to the patient's job or sport.
- Proprioception: Exercises are designed to correct a "distorted body schema" or altered mental representation of the back that can result from chronic pain and surgery.
- Return-to-Activity Planning: Multidisciplinary programs, particularly those coordinated with medical advisors, significantly increase the probability of a faster return to work.
4. Ongoing Education and Self-Management
Long-term success relies on the patient’s ability to maintain spinal health and prevent recurrence.
- Ergonomics and Mechanics: Ongoing training focuses on body mechanics and ergonomics to protect the spine during work and daily life.
- Load Management: Patients learn strategies to pace their activities and manage physical loads to avoid recurring strain.
- Prevention of Re-herniation: While recurrent herniation affects 3% to 12% of patients, active rehabilitation does not increase this risk; instead, it prevents the long-term "muscular burden" caused by inactivity.
- Adherence Challenges: Because back muscle strength may decrease for up to three months post-operatively without intervention, and adherence to home programs often drops significantly after two months, a long-term conditioning program is essential.
Preventing Recurrence After Discectomy
Preventing recurrence after a lumbar discectomy—which occurs in 3% to 12% of patients—is a primary goal of postoperative management. Source emphasize that active rehabilitation does not increase the risk of re-herniation or reoperation and is essential for counteracting the "muscular burden" caused by post-surgical inactivity.
Strategies for Long-Term Prevention
Based on source, effective prevention relies on a combination of physical conditioning, movement modification, and consistent activity:
- Consistent Core Strengthening: Rehabilitation programs that emphasize lumbar stabilization and motor control exercises are critical for restoring the function of deep stabilizers like the lumbar multifidus (LM) and transversus abdominis (TrA). These muscles provide approximately two-thirds of the stability at the L4-L5 segment, and their failure to automatically recover after surgery can lead to persistent dysfunction and recurring pain.
- Proper Mechanics and Posture: Patient education focuses heavily on maintaining a neutral lumbar lordosis and using safe strategies for activities of daily living. This includes training on lifting techniques and "correct working posture" to protect the healing spinal tissues from excessive stress.
- Managing Lumbar Flexion: Some evidence-based protocols recommend focusing on extension exercises and limiting repetitive flexion (bending forward) during the early phases of recovery to protect the surgical site. However, research also shows that for low-risk patients, lifting activity restrictions as early as two weeks post-surgery can shorten sick leave without increasing complication rates.
- Movement Breaks from Sitting: To address stiffness, some clinical instructions specifically recommend performing extension exercises after prolonged periods of sitting or flexion.
- Regular Walking and Aerobic Fitness: Daily walking is encouraged to improve circulation and cardiovascular health. A 12-week walking program has been shown to increase oxygen consumption and training effects without increasing a patient's pain level.
- Addressing Stiffness with Mobility Work: Restoring a full range of motion is vital, as lumbar spine mobility is typically restricted to 60% of normal levels three months after a disc excision. Rehabilitation uses stretching and joint mobilization to prevent long-term spinal dysfunction.
- Overall Conditioning and Load Management: Advanced rehabilitation incorporates high-intensity exercise and global strengthening of the pelvic, hip, and trunk muscles. These intensive programs lead to a faster decrease in pain and disability and a quicker return to work compared to low-intensity care.
The Role of Long-Term Adherence
A significant challenge in preventing recurrence is that adherence to home exercise programs often drops to 30–50% after the first few months. Because muscle strength may continue to decrease until three months post-operatively, a long-term commitment to a conditioning program is necessary to maintain functional health states for a decade or more
Our Specialized Approach to Rehabilitation
- Nerve and Mobility Assessment: Your focus on assessing nerve and mobility recovery is supported by clinical protocols that use the straight leg raise (SLR) test to monitor neural tension and kypheometry or inclinometry to measure the range of motion of the trunk. Some specialized approaches also utilize rehabilitative ultrasound imaging (RUSI) to objectively quantify the recovery of muscle activation in the deep stabilizers.
- Individualized Stabilization Programs: The sources emphasize the critical role of lumbar stabilization exercises, particularly those targeting the transversus abdominis (TrA) and lumbar multifidus (LM). These muscles often exhibit atrophy or delayed activation following surgery, and individualized programs are necessary because recovery of these structures is not automatic after the resolution of pain.
- Manual Therapy and Surgical Healing: Your inclusion of manual therapy techniques is consistent with protocols that utilize joint and soft-tissue mobilization as adjuncts to exercise. Specialized techniques like neural mobilization (nerve gliding) are also used to reduce local edema and maintain the "gliding" of neural structures during the healing phase.
- Progressive Strength and Flexibility Training: Evidence indicates that progressive programs—transitioning from gentle mobilization to high-intensity strengthening—lead to a faster decrease in pain and disability than low-intensity care. Effective protocols often utilize sustained isometric contractions to increase the endurance of trunk muscles while minimizing potentially harmful shear loading of the spine.
- Education for Autonomy and Confidence: Patient education is considered one of the most vital early interventions. Teaching neutral lumbar lordosis, safe body mechanics (like "log-rolling" out of bed), and activity pacing helps to manage patient expectations and reduce kinesiophobia (fear of movement), which is a significant barrier to functional recovery.
- Surgical Team Collaboration: Regular communication between rehabilitation and surgical teams ensures that activity progression respects tissue healing timelines—such as waiting for bony fusion or ensuring the surgical site is stable before starting intensive resistance training. Multidisciplinary rehabilitation that includes early contact with medical advisors has been shown to result in a faster return to work
FAQs
- Will my leg pain improve right away?
- Often, yes. Most patients experience substantial relief of leg symptoms shortly after surgery, as the primary goal of the procedure is to decompress the pinched nerve. The reported success rate for lumbar disc surgery is high, ranging from 78% to 95% at one to two years post-operation. However, it is important to note that 22% to 45% of patients may experience some level of residual sciatica (leg pain). Sensations like numbness or tingling can take longer to resolve as the nerve heals
- Is back pain normal after discectomy?
- Yes. Between 30% and 70% of patients report residual back pain following the procedure. In the early weeks, this is typically due to incisional discomfort and muscular factors. Research shows that back muscle strength often continues to decrease for up to three months post-operatively before beginning to improve through targeted rehabilitation [7, 79, History].
- When can I return to work?Return-to-work timelines depend on the physical demands of your job and the intensity of your recovery program:
- Light Duties: Patients who participate in immediate physiotherapy have been shown to return to work in a median of 6 weeks, compared to 8 weeks for those receiving standard care.
- Heavier Jobs: Research on intensive exercise programs found that participants returned to work after an average of 56 days (8 weeks), while those in lower-intensity programs took roughly 75 days (11 weeks).
- Medical Guidance: Multidisciplinary programs involving coordination with medical advisors have been proven to result in a significantly faster return to work
- Can the disc re-herniate?
- Yes, though it is relatively uncommon. Recurrent herniation is estimated to occur in 3% to 12% of patients who have had their first disc surgery. Crucially, sources emphasize that active exercise and rehabilitation do not increase the risk of re-herniation or reoperation. Instead, programs that focus on lumbar stabilization and re-training core muscles like the multifidus are recommended to protect the spine and reduce the risk of future issues.
- When can I exercise again?
- Immediately: Patients are often encouraged to begin gradual mobilization, such as gentle walking and simple knee/hip flexion, within two hours to one day after surgery.
- 2–4 Weeks: In low-risk patients, lifting activity restrictions as early as two weeks post-surgery has been shown to be safe and can shorten sick leave. Formal motor control exercises to re-train deep stabilizers can also be initiated within this window, sometimes as early as 10 days post-op.
- 4–6 Weeks: This is the most common timeframe for starting a structured, supervised therapeutic exercise program
Take the First Step Toward Recovery
Don't let a discectomy limit your activities or affect your daily life. Our experienced team is ready to help you build a strong foundation for lasting recovery.
Book Your Specialized Assessment Today:
Phone: 905-669-1221
Location: 398 Steeles Ave W #201, Thornhill, ON L4J 6X3
Online Booking: www.vaughanphysiotherapy.com
Serving communities across Thornhill, Langstaff, Newtonbrook, Willowdale, North York, Markham, Richmond Hill, Concord, and North Toronto.
Conveniently located in the heart of Thornhill, offering flexible scheduling to accommodate your recovery needs.
Created by Sara Lam