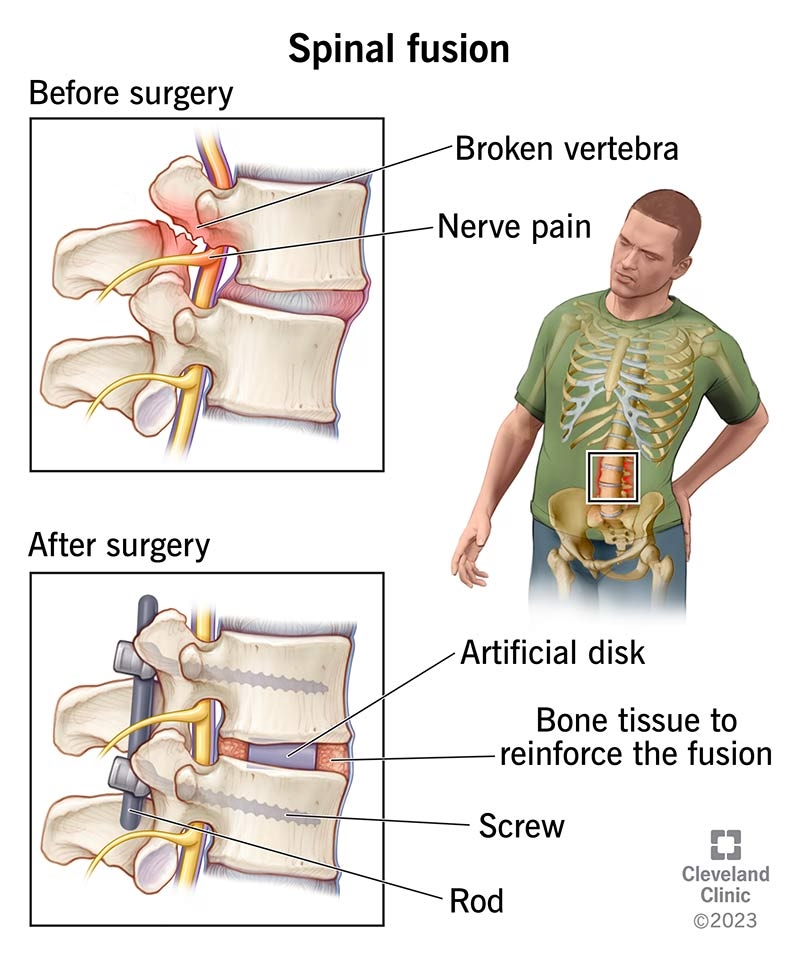
Why Physiotherapy Is Critical for Lumbar Fusion Recovery
Physiotherapy is essential for recovery because clinical outcomes often lag behind surgical success; statistics from the Swedish National Spine Register show that 25% of patients experience unimproved or worsened pain and up to 40% are dissatisfied 12 months after a lumbar fusion. Structured rehabilitation addresses the physical and psychological barriers that surgery alone cannot resolve.
Ensuring Safe Early Healing
Contrary to historical concerns, research demonstrates that postoperative rehabilitation can be safely implemented within the first three months after fusion. Early exercise has been shown not to overload lumbar internal fixation, and immediate mobilization—such as supervised gait and transfer training in the acute care setting—can reduce adverse events and shorten your length of hospital stay.
Restoring Motor Control and Core Stability
A primary goal of physiotherapy is to re-activate deep stabilizers like the lumbar multifidus (LM) and transversus abdominis (TrA).
- Non-Automatic Recovery: Weakness and atrophy of these muscles are nearly universal after spinal injury and surgery, and recovery is not automatic even after pain has been resolved.
- The "Splinting Effect": Targeted neutral spine control exercises promote a "splinting effect" through the cocontraction of abdominal and extensor muscles, which protects the healing spine during functional tasks like lifting and bending.
Protecting Adjacent Segments
Because fusion eliminates motion at a specific level, it alters overall spinal kinematics and can increase mechanical stress on the segments above and below.
- Compensatory Mobility: Physiotherapy focuses on optimizing the mobility of musculoskeletal units cranial (thoracic spine) and caudal (hips) to the fusion. Improving rotation in the thoracic spine and flexibility in the hips helps maintain proper posture and decreases torsional stress on the healing fusion.
- Stabilization: Proper motor control training is theorized to decrease a patient's long-term risk for adjacent-segment pathologies by providing better dynamic support.
The "Complex Rehabilitation" Advantage
Sources highlight that "complex" or "psychomotor" therapy—which combines physical exercise with Cognitive Behavioral Therapy (CBT)—is significantly more effective than standard exercise alone.
- Functional Gains: This approach produces clinically meaningful reductions in disability and pain-related fear.
- Return to Activity: Patients who undergo psychomotor therapy show higher employment levels and significantly less long-term sickness leave compared to those who follow basic home exercise programs.
Consequences of Inadequate Rehabilitation
Without proper intervention, the interaction between physical tissue disruption and psychosocial factors can lead to a cycle of chronic pain. Chronic inactivity leads to local denervation atrophy of the paraspinal muscles, which is strongly associated with inferior clinical outcomes. Furthermore, failing to address kinesiophobia (fear of movement) can prevent patients from ever returning to their prior levels of physical demand
What to Expect: Prognosis and Recovery Timeline
The recovery timeline following lumbar fusion is a progressive process that requires a balance between protecting the healing bone graft and restoring the function of disrupted tissues. While surgical success is common, approximately 25% of patients report static or worsening pain, and up to 40% are dissatisfied at the 12-month mark, highlighting the importance of a structured rehabilitation pathway.
0–6 Weeks: Protection Phase
The primary focus during the first month and a half is surgical site protection and the initiation of basic mobility.
- Immediate Mobilization: Modern evidence supports immediate mobilization (gait and transfer training) in the hospital to reduce adverse events and shorten the length of stay.
- Early Walking and Education: Patients are encouraged to begin a walking program immediately to facilitate circulation and cardiovascular health. Education focuses on neutral lumbar posture and avoiding excessive "outer-range" spinal movements to protect internal fixation.
- Core Activation: Formal lumbopelvic stabilization—specifically targeting the transversus abdominis (TrA) and lumbar multifidus (LM) through gentle contractions—can safely begin as early as the first few weeks post-surgery.
6–12 Weeks: Early Strength Phase
This stage marks the transition from simple protection to active muscle re-education.
- Formal Rehabilitation Window: While some early exercises begin sooner, many experts recommend starting formal, supervised neutral spine rehabilitation at 8 to 12 weeks to align with bony tissue healing. Interestingly, starting rehabilitation at 12 weeks has been shown to result in better clinical outcomes and lower costs than a 6-week start.
- Targeting Deep Stabilizers: This phase emphasizes motor control training to address the atrophy and denervation of paraspinal muscles common after fusion surgery. Exercises typically progress to closed kinetic chain activities, such as wall-supported semi-squats and step-ups.
- Compensatory Mobility: To reduce stress on the healing fusion, therapists focus on improving the mobility of the thoracic spine and hips, which prevents the "overload" of adjacent segments.
3–6 Months: Functional Phase
As the fusion begins to stabilize, rehabilitation shifts toward restoring daily autonomy and global strength.
- Advanced Functional Training: Exercises progress to more complex movements, including forward lunges and step-ups with elevated arms, to integrate stabilization with functional loading.
- Body Mechanics Retraining: This period is critical for retraining safe lifting, bending, and transfer strategies, using core co-contractions to provide a "splinting effect" for the spine.
- Return to Work: Patients participating in "complex rehabilitation" (combining exercise with cognitive-behavioral strategies) show significantly higher employment levels and less long-term sickness leave compared to those receiving standard exercise advice.
6–12 Months: Full Activity Phase
The final stage of recovery involves a gradual return to the patient's pre-surgical physical demands.
- Stabilization and Impact: While walking starts early, higher-impact activities like running or contact sports are generally restricted for at least the first six months to ensure the fusion site has fully matured.
- Long-Term Conditioning: Full recovery can take a year or longer, as back muscle strength and density often lag significantly behind the resolution of acute pain.
- Psychological Readiness: Success in this phase is often determined by the reduction of kinesiophobia (fear of movement). Programs that address "maladaptive pain cognitions" alongside physical training result in a more successful return to dynamic sports and heavy lifting
Physiotherapy Treatment Approaches
Physiotherapy treatment after lumbar fusion is a multidimensional process that integrates physical conditioning with psychological support to address the surgical disruption of tissues and the loss of segmental motion. Evidence suggests that "complex rehabilitation"—which combines exercise with cognitive-behavioral strategies—is significantly more effective than exercise alone in reducing long-term disability and fear of movement.
1. Education and Cognitive Support
Patient education is considered the cornerstone of rehabilitation.
- Movement Precautions: Early education focuses on maintaining a neutral lumbar lordosis and avoiding outer-range lumbar movements, contact sports, or heavy lifting for the first six months to protect internal fixation.
- Psychological Coping: Specialized "psychomotor" therapy includes sessions on modifying maladaptive pain cognitions, relaxation techniques, and managing "flare-ups" to increase self-efficacy and reduce kinesiophobia (fear of movement).
2. Early Mobilization and Gait Retraining
- Acute Phase: Immediate mobilization, including supervised gait and transfer training, is initiated in the hospital to reduce adverse events and shorten the length of stay.
- Normalization: Walking is encouraged immediately as a primary form of cardiovascular exercise, with the expectation of a gradual increase in frequency and distance as symptoms allow.
3. Core Stabilization and Motor Control
Re-activating the deep stabilizers is critical because these muscles often exhibit atrophy and denervation following the surgical approach.
- Neutral Spine Control: Exercises target the transversus abdominis (TrA) and lumbar multifidus (LM) through isolated cocontractions while maintaining a neutral posture.
- Splinting Effect: Proper activation of these muscles provides a "splinting effect" that protects the healing spine during functional loading.
4. Mobility and Movement Training
- Compensatory Mobility: Because the fused level has lost motion, rehabilitation focuses on optimizing the mobility of musculoskeletal units cranial (thoracic spine) and caudal (hips) to the fusion.
- Reducing Stress: Thoracic rotation training and hip mobilization are used to maintain proper posture and decrease torsional stress on the healing fusion and adjacent segments.
- Neural Mobility: While evidence for its superiority is contested, nerve mobilization (nerve glides) is often included to improve range of motion and prevent nerve roots from adhering to scar tissue.
5. Progressive Strengthening and Function
- Functional Strength: Programs progress from isolated contractions to closed kinetic chain exercises like wall-supported semi-squats, side lunges, and step-ups.
- Gluteal and Leg Power: Strengthening the glutes, hamstrings, and quadriceps is essential for supporting the spine during daily tasks like rising from a chair or climbing stairs.
- Advanced Training: Later stages (9–12 weeks) integrate stabilization with open kinetic chain exercises, such as unsupported leg cycling or four-point kneeling exercises with arm and leg extensions.
6. Postural, Ergonomic, and Cardiovascular Conditioning
- Ergonomics: Training includes ergonomic directions for returning to work and managing daily physical loads.
- Aerobic Fitness: Cardiovascular fitness is typically maintained through a walking program or stationary cycling, which has been shown to improve long-term health without increasing back pain.
Timing and Tailoring
While education and walking begin immediately, formal outpatient neutral spine rehabilitation is often recommended to begin at 12 weeks postoperatively to align with bony tissue healing timeframes. Starting at 12 weeks has been associated with better outcomes at a lower cost than starting earlier at 6 weeks
Preventing Post-Fusion Complications and Recurrence of Pain
Preventing complications and the recurrence of pain after a lumbar fusion requires a comprehensive approach that addresses both the physical structural changes and the psychological factors associated with chronic spinal conditions. While surgical success rates for stabilization are high, approximately 25% of patients report unimproved or worsened pain 12 months post-operation, making long-term self-management essential.
Physical Strategies for Long-Term Health
- Strengthening Core and Hip Muscles: Sustained exercise is vital because the deep paraspinal muscles, particularly the lumbar multifidus, often exhibit significant atrophy and denervation following the surgical approach. These muscles do not automatically recover after surgery, and their weakness is correlated with inferior clinical outcomes. Rehabilitation focusing on lumbopelvic stabilization (targeting the transversus abdominis and multifidus) provides a "splinting effect" that protects the healing spine.
- Movement Mechanics and Mobility: To compensate for the loss of motion at the fused segment, it is critical to improve the mobility of the thoracic spine and hips. This prevents the "overload" of adjacent vertebrae and decreases torsional stress on the healing fusion. Standard protocols recommend avoiding outer-range lumbar movements and heavy lifting for at least the first six months.
- Walking and Cardiovascular Fitness: Regular aerobic activity, specifically walking, is recommended to improve long-term health without increasing back pain symptoms. Preoperative cardiovascular exercise has even been shown to decrease hospital length of stay and improve post-operative functional scores.
Critical Lifestyle and Behavioral Factors
- Smoking Cessation: Avoiding smoking is explicitly identified as critical for long-term success, as it is a strong predictor of worse clinical outcomes and can hinder the fusion process.
- Addressing Pain-Related Fear: A major factor in the recurrence of pain is kinesiophobia (fear of movement) and pain catastrophizing. Patients who develop a fear of re-injury often remain inactive, leading to further deconditioning and chronic disability.
- The "Complex Rehabilitation" Advantage: Evidence shows that "complex rehabilitation"—which combines physical exercise with Cognitive Behavioral Therapy (CBT)—is significantly more effective at reducing long-term disability and fear-avoidance behavior than exercise alone. This approach helps patients modify maladaptive pain cognitions and increases their confidence in returning to full activity.
Preventing Deconditioning
Pre-operative and post-operative deconditioning are significant risk factors for poor recovery. Because trunk muscle strength may continue to decrease for months after the procedure, maintaining a consistent, long-term strengthening routine is the most effective strategy for reducing future low back pain and preventing adjacent-segment pathologies
Our Specialized Approach to Rehabilitation
Phase-Based and Surgeon-Aligned Protocols
Evidence supports a structured, phase-based progression that respects tissue healing while promoting early activity:
- Early Protection (0–6 Weeks): Initial care focuses on respiratory/circulatory exercises, transfer training, and a walking program. Clinical guidelines suggest that "prehabilitation" and early mobilization (starting as early as postoperative day 1) can shorten hospital stays and improve early functional scores.
- Formal Rehabilitation (12 Weeks): High-level evidence recommends beginning formal, outpatient neutral spine rehabilitation at 12 weeks post-surgery. This delay aligns with bony tissue healing and has been shown to result in better outcomes at a lower cost than an earlier 6-week start.
Evidence-Based Strengthening and Resiliency
Your focus on core and hip strengthening is critical for protecting the fusion and adjacent segments:
- Lumbopelvic Stabilization: Training targets the transversus abdominis and lumbar multifidus through specific cocontractions. This provides a "splinting effect" that protects the spine during functional loading.
- Addressing Muscle Morbidity: Surgery and pre-existing pain lead to muscle denervation and atrophy in the paraspinal muscles; because recovery is not automatic, targeted motor control exercises are essential to restore core strength.
- Compensatory Mobility: To prevent adjacent-segment pathologies, rehabilitation optimizes the mobility of the thoracic spine and hips, which reduces torsional stress on the healing fusion site.
Individualized Pacing and Psychosocial Support
A "psychomotor" or "complex rehabilitation" approach—combining exercise with cognitive-behavioral therapy (CBT)—is significantly more effective than exercise alone.
- Preventing Flare-Ups: Individualized pacing and cognitive coping strategies help patients manage setbacks and flare-ups without retreating into inactivity.
- Building Confidence: This approach specifically targets kinesiophobia (fear of movement) and catastrophizing, which are present in approximately 80% of fusion patients and are strong predictors of poor outcomes.
Safe Progression and Collaborative Communication
- Milestones and Restrictions: Standard protocols restrict heavy lifting, contact sports, and outer-range lumbar movements for the first 6 months to ensure the fusion stabilizes.
- Multidisciplinary Alignment: Collaborative care and case management involving the surgical team are recommended to coordinate expectations, improve patient satisfaction, and facilitate a faster return to work.
- Monitoring Red Flags: While early rehabilitation is proven safe and does not overload internal fixation, close monitoring is necessary to ensure reoperation rates remain within normal clinical ranges
FAQs
- Is pain normal after lumbar fusion?
- Yes, post-surgical pain and stiffness are common. While the procedure aims to reduce pain, statistics from the Swedish National Spine Register indicate that 25% of patients experience unimproved or even worsened back and/or leg pain at the 12-month mark. Residual symptoms are often attributed to the surgical disruption of tissues, such as the denervation and atrophy of paraspinal muscles, or nerve root adherence to scar tissue. However, these symptoms generally improve with structured rehabilitation that includes CBT (Cognitive Behavioral Therapy) to manage pain-related fear and "catastrophizing"
- When can I start physiotherapy?Physiotherapy typically begins in two stages:
- Immediate Mobilization: Education, breathing exercises, and a walking program should begin immediately following surgery in the acute care setting to reduce adverse events and shorten hospital stays.
- Formal Rehabilitation: While some protocols initiate motor control exercises as early as 0–3 weeks post-surgery, high-level evidence suggests that starting formal, outpatient "neutral spine" rehabilitation at the 12-week mark results in better clinical outcomes at a lower cost than an earlier 6-week start
- When can I return to work?
- Return-to-work timelines are highly individualized and depend on the intensity of your rehabilitation. Patients who participate in "complex rehabilitation" (combining exercise with cognitive-behavioral strategies) show significantly higher employment levels and lower rates of long-term sickness leave (longer than 6 months) compared to those receiving standard exercise advice. Research indicates that patients in these intensive programs have a faster return to work, while those who were off work for more than 13 weeks prior to surgery may face a more challenging recovery
- Will the fusion limit my mobility?
- Yes, the specific segment that is fused will no longer move. This "segmental immobilization" is a direct intended result of the surgery to provide stability. To compensate for this loss of motion, rehabilitation focuses on optimizing the mobility of the thoracic spine and hips. Improving flexibility in these areas helps you maintain proper posture and perform daily activities without putting excessive stress on the healing fusion site
- Can other spinal levels wear out?
- There is a recognized risk of adjacent-segment pathology, where the vertebrae immediately above or below the fusion site experience increased mechanical stress. One study reported adjacent level degeneration requiring further surgery in 1.9% to 3.8% of patients within 2–3 years. To mitigate this risk, physiotherapy emphasizes core stabilization exercises and functional movement training to provide dynamic support for the spine and distribute loads more effectively
Take the First Step Toward Recovery
Don't let a lumbar fusion limit your activities or affect your daily life. Our experienced team is ready to help you build a strong foundation for lasting recovery.
Book Your Specialized Assessment Today:
Phone: 905-669-1221
Location: 398 Steeles Ave W #201, Thornhill, ON L4J 6X3
Online Booking: www.vaughanphysiotherapy.com
Serving communities across Thornhill, Langstaff, Newtonbrook, Willowdale, North York, Markham, Richmond Hill, Concord, and North Toronto.
Conveniently located in the heart of Thornhill, offering flexible scheduling to accommodate your recovery needs.
Created by Sara Lam
.avif)